For more information, visit http://www.nhlbi.nih.gov/health/health-topics/topics/hbc/
What Is Cholesterol?
To understand high blood cholesterol (ko-LES-ter-ol), it helps to learn about cholesterol. Cholesterol is a waxy, fat-like substance that’s found in all cells of the body.
Your body needs some cholesterol to make hormones, vitamin D, and substances that help you digest foods. Your body makes all the cholesterol it needs. However, cholesterol also is found in some of the foods you eat.
Cholesterol travels through your bloodstream in small packages called lipoproteins (lip-o-PRO-teens). These packages are made of fat (lipid) on the inside and proteins on the outside.
Two kinds of lipoproteins carry cholesterol throughout your body: low-density lipoproteins (LDL) and high-density lipoproteins (HDL). Having healthy levels of both types of lipoproteins is important.
LDL cholesterol sometimes is called “bad” cholesterol. A high LDL level leads to a buildup of cholesterol in your arteries. (Arteries are blood vessels that carry blood from your heart to your body.)
HDL cholesterol sometimes is called “good” cholesterol. This is because it carries cholesterol from other parts of your body back to your liver. Your liver removes the cholesterol from your body.
What Is High Blood Cholesterol?
High blood cholesterol is a condition in which you have too much cholesterol in your blood. By itself, the condition usually has no signs or symptoms. Thus, many people don’t know that their cholesterol levels are too high.
People who have high blood cholesterol have a greater chance of getting coronary heart disease, also called coronary artery disease. (In this article, the term “heart disease” refers to coronary heart disease.)
The higher the level of LDL cholesterol in your blood, the GREATER your chance is of getting heart disease. The higher the level of HDL cholesterol in your blood, the LOWER your chance is of getting heart disease.
Coronary heart disease is a condition in which plaque (plak) builds up inside the coronary (heart) arteries. Plaque is made up of cholesterol, fat, calcium, and other substances found in the blood. When plaque builds up in the arteries, the condition is called atherosclerosis (ATH-er-o-skler-O-sis).
Atherosclerosis
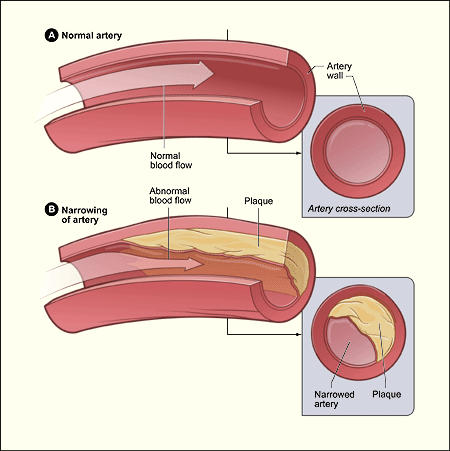
Figure A shows a normal artery with normal blood flow. The inset image shows a cross-section of a normal artery. Figure B shows an artery with plaque buildup. The inset image shows a cross-section of an artery with plaque buildup.
Over time, plaque hardens and narrows your coronary arteries. This limits the flow of oxygen-rich blood to your heart muscle.
Eventually, an area of plaque can rupture (break open). This causes a blood clot to form on the surface of the plaque. If the clot becomes large enough, it can mostly or completely block blood flow through a coronary artery.
If the flow of oxygen-rich blood to your heart muscle is reduced or blocked, angina (an-JI-nuh or AN-juh-nuh) or a heart attack may occur.
Angina is chest pain or discomfort. It may feel like pressure or squeezing in your chest. The pain also may occur in your shoulders, arms, neck, jaw, or back. Angina pain may even feel like indigestion.
A heart attack occurs if the flow of oxygen-rich blood to a section of heart muscle suddenly becomes blocked. If blood flow isn’t restored quickly, the section of heart muscle begins to die. Without quick treatment, a heart attack can lead to serious problems and even death.
Plaque also can build up in other arteries in your body, such as the arteries that bring oxygen-rich blood to your brain and limbs. This can lead to problems such as carotid artery disease, stroke, and peripheral arterial disease (P.A.D.).
Outlook
Lowering your cholesterol may slow, reduce, or even stop the buildup of plaque in your arteries. It also may reduce the risk of plaque rupturing and causing dangerous blood clots.
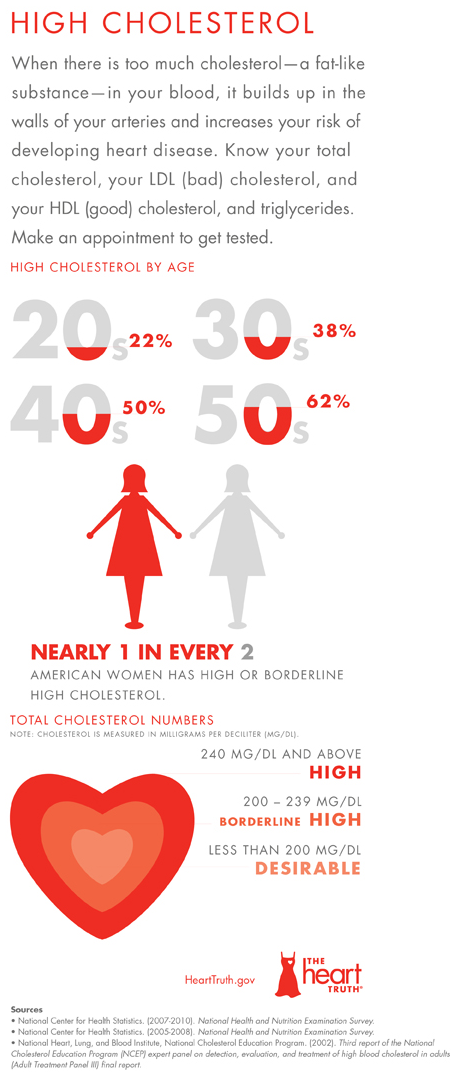
The image focuses on high cholesterol in women and explains how high cholesterol increases the risk of developing heart disease. An estimated 1 in 2 women has high or borderline high cholesterol.
The image also lists the ranges of total cholesterol numbers for high, borderline high, and desirable cholesterol levels, and breaks down the percentage of women who have high cholesterol in their twenties, thirties, forties, and fifties.
Sources: National Center for Health Statistics (2007–2010). National Health and Nutrition Examination Survey; National Center for Health Statistics (2005–2008). National Health and Nutrition Examination Survey; National Heart, Lung, and Blood Institute, National Cholesterol Education Program (2002). Third report of the National Cholesterol Education Program (NCEP) exert panel on detection, evaluation, and treatment of high blood cholesterol in adults (Adult Treatment Panel III) final report.
Other Names for High Blood Cholesterol
- Hypercholesterolemia (HI-per-ko-LES-ter-ol-E-me-ah)
- Hyperlipidemia (HI-per-lip-ih-DE-me-ah)
What Causes High Blood Cholesterol?
Many factors can affect the cholesterol levels in your blood. You can control some factors, but not others.
Factors You Can Control
Diet
Cholesterol is found in foods that come from animal sources, such as egg yolks, meat, and cheese. Some foods have fats that raise your cholesterol level.
For example, saturated fat raises your low-density lipoprotein (LDL) cholesterol level more than anything else in your diet. Saturated fat is found in some meats, dairy products, chocolate, baked goods, and deep-fried and processed foods.
Trans fatty acids (trans fats) raise your LDL cholesterol and lower your high-density lipoprotein (HDL) cholesterol. Trans fats are made when hydrogen is added to vegetable oil to harden it. Trans fats are found in some fried and processed foods.
Limiting foods with cholesterol, saturated fat, and trans fats can help you control your cholesterol levels.
Physical Activity and Weight
Lack of physical activity can lead to weight gain. Being overweight tends to raise your LDL level, lower your HDL level, and increase your total cholesterol level. (Total cholesterol is a measure of the total amount of cholesterol in your blood, including LDL and HDL).
Routine physical activity can help you lose weight and lower your LDL cholesterol. Being physically active also can help you raise your HDL cholesterol level.
Factors You Can’t Control
Heredity
High blood cholesterol can run in families. An inherited condition called familial hypercholesterolemia causes very high LDL cholesterol. (“Inherited” means the condition is passed from parents to children through genes.) This condition begins at birth, and it may cause a heart attack at an early age.
Age and Sex
Starting at puberty, men often have lower levels of HDL cholesterol than women. As women and men age, their LDL cholesterol levels often rise. Before age 55, women usually have lower LDL cholesterol levels than men. However, after
age 55, women can have higher LDL levels than men.
What Are the Signs and Symptoms of High Blood Cholesterol?
High blood cholesterol usually has no signs or symptoms. Thus, many people don't know that their cholesterol levels are too high.
If you're 20 years old or older, have your cholesterol levels checked at least once every 5 years. Talk with your doctor about how often you should be tested.
How Is High Blood Cholesterol Diagnosed?
Your doctor will diagnose high blood cholesterol by checking the cholesterol levels in your blood. A blood test called a lipoprotein panel can measure your cholesterol levels. Before the test, you’ll need to fast (not eat or drink anything but water) for
The lipoprotein panel will give your doctor information about your:
- Total cholesterol. Total cholesterol is a measure of the total amount of cholesterol in your blood, including low-density lipoprotein (LDL) cholesterol and high-density lipoprotein (HDL) cholesterol.
- LDL cholesterol. LDL, or “bad,” cholesterol is the main source of cholesterol buildup and blockages in the arteries.
- HDL cholesterol. HDL, or “good,” cholesterol helps remove cholesterol from your arteries.
- Triglycerides (tri-GLIH-seh-rides). Triglycerides are a type of fat found in your blood. Some studies suggest that a high level of triglycerides in the blood may raise the risk of coronary heart disease, especially in women.
If it’s not possible to have a lipoprotein panel, knowing your total cholesterol and HDL cholesterol can give you a general idea about your cholesterol levels.
Testing for total and HDL cholesterol does not require fasting. If your total cholesterol is 200 mg/dL or more, or if your HDL cholesterol is less than 40 mg/dL, your doctor will likely recommend that you have a lipoprotein panel. (Cholesterol is measured as milligrams (mg) of cholesterol per deciliter (dL) of blood.)
The tables below show total, LDL, and HDL cholesterol levels and their corresponding categories. See how your cholesterol numbers compare to the numbers in the tables below.
| Total Cholesterol Level | Total Cholesterol Category |
|---|---|
| Less than 200 mg/dL | Desirable |
| 200–239 mg/dL | Borderline high |
| 240 mg/dL and higher | High |
| LDL Cholesterol Level | LDL Cholesterol Category |
|---|---|
| Less than 100 mg/dL | Optimal |
| 100–129 mg/dL | Near optimal/above optimal |
| 130–159 mg/dL | Borderline high |
| 160–189 mg/dL | High |
| 190 mg/dL and higher | Very high |
| HDL Cholesterol Level | HDL Cholesterol Category |
|---|---|
| Less than 40 mg/dL | A major risk factor for heart disease |
| 40–59 mg/dL | The higher, the better |
| 60 mg/dL and higher | Considered protective against heart disease |
Triglycerides also can raise your risk for heart disease. If your triglyceride level is borderline high (150–199 mg/dL) or high (200 mg/dL or higher), you may need treatment.
Factors that can raise your triglyceride level include:
- Overweight and obesity
- Lack of physical activity
- Cigarette smoking
- Excessive alcohol use
- A very high carbohydrate diet
- Certain diseases and medicines
- Some genetic disorders
How Is High Blood Cholesterol Treated?
High blood cholesterol is treated with lifestyle changes and medicines. The main goal of treatment is to lower your low-density lipoprotein (LDL) cholesterol level enough to reduce your risk for coronary heart disease, heart attack, and other related health problems.
Your risk for heart disease and heart attack goes up as your LDL cholesterol level rises and your number of heart disease risk factors increases.
Some people are at high risk for heart attacks because they already have heart disease. Other people are at high risk for heart disease because they have diabetes or more than one heart disease risk factor.
Talk with your doctor about lowering your cholesterol and your risk for heart disease. Also, check the list to find out whether you have risk factors that affect your LDL cholesterol goal:
- Cigarette smoking
- High blood pressure (140/90 mmHg or higher), or you’re on medicine to treat high blood pressure
- Low high-density lipoprotein (HDL) cholesterol (less than 40 mg/dL)
- Family history of early heart disease (heart disease in father or brother before age 55; heart disease in mother or sister before age 65)
- Age (men 45 years or older; women 55 years or older)
You can use the NHLBI 10-Year Risk Calculator to find your risk score. The score, given as a percentage, refers to your chance of having a heart attack in the next 10 years.
Based on your medical history, number of risk factors, and risk score, figure out your risk of getting heart disease or having a heart attack using the table below.
| If You Have | You Are in Category | Your LDL Goal Is |
|---|---|---|
| Heart disease, diabetes, or a risk score higher than 20% | I. High risk* | Less than 100 mg/dL |
| Two or more risk factors and a risk score of | II. Moderately high risk | Less than 130 mg/dL |
| Two or more risk factors and a risk score lower than 10% | III. Moderate risk | Less than 130 mg/dL |
| One or no risk factors | IV. Low to moderate risk | Less than 160 mg/dL |
*Some people in this category are at very high risk because they’ve just had a heart attack or they have diabetes and heart disease, severe risk factors, or metabolic syndrome. If you’re at very high risk, your doctor may set your LDL goal even lower, to less than 70 mg/dL. Your doctor also may set your LDL goal at this lower level if you have heart disease alone.
After following the above steps, you should have an idea about your risk for heart disease and heart attack. The two main ways to lower your cholesterol (and, thus, your heart disease risk) include:
- Therapeutic Lifestyle Changes (TLC). TLC is a three-part program that includes a healthy diet, weight management, and physical activity. TLC is for anyone whose LDL cholesterol level is above goal.
- Medicines. If cholesterol-lowering medicines are needed, they’re used with the TLC program to help lower your LDL cholesterol level.
Your doctor will set your LDL goal. The higher your risk for heart disease, the lower he or she will set your LDL goal. Using the following guide, you and your doctor can create a plan for treating your high blood cholesterol.
Category I, high risk, your LDL goal is less than 100 mg/dL.*
| Your LDL Level | Treatment |
|---|---|
| If your LDL level is 100 or higher | You will need to begin the TLC diet and take medicines as prescribed. |
| Even if your LDL level is below 100 | You should follow the TLC diet to keep your LDL level as low as possible. |
* Your LDL goal may be set even lower, to less than 70 mg/dL, if you’re at very high risk or if you have heart disease. If you have this lower goal and your LDL is 70 mg/dL or higher, you’ll need to begin the TLC diet and take medicines as prescribed.
Category II, moderately high risk, your LDL goal is less than 130 mg/dL.
| Your LDL Level | Treatment |
|---|---|
| If your LDL level is 130 mg/dL or higher | You will need to begin the TLC diet. |
| If your LDL level is 130 mg/dL or higher after 3 months on the TLC diet | You may need medicines along with the TLC diet. |
| If your LDL level is less than | You will need to follow a heart healthy diet. |
Category III, moderate risk, your LDL goal is less than 130 mg/dL.
| Your LDL Level | Treatment |
|---|---|
| If your LDL level is 130 mg/dL or higher | You will need to begin the TLC diet. |
| If your LDL level is 160 mg/dL or higher after 3 months on the TLC diet | You may need medicines along with the TLC diet. |
| If your LDL level is less than | You will need to follow a heart healthy diet. |
Category IV, low to moderate risk, your LDL goal is less than 160 mg/dL.
| Your LDL Level | Treatment |
|---|---|
| If your LDL level is 160 mg/dL or higher | You will need to begin the TLC diet. |
| If your LDL level is 160 mg/dL or higher after 3 months on the TLC diet | You may need medicines along with the TLC diet. |
| If your LDL level is less than | You will need to follow a heart healthy diet. |
Lowering Cholesterol Using Therapeutic Lifestyle Changes
TLC is a set of lifestyle changes that can help you lower your LDL cholesterol. The main parts of the TLC program are a healthy diet, weight management, and physical activity.
The TLC Diet
With the TLC diet, less than 7 percent of your daily calories should come from saturated fat. This kind of fat is found in some meats, dairy products, chocolate, baked goods, and deep-fried and processed foods.
No more than 25 to 35 percent of your daily calories should come from all fats, including saturated, trans, monounsaturated, and polyunsaturated fats.
You also should have less than 200 mg a day of cholesterol. The amounts of cholesterol and the types of fat in prepared foods can be found on the foods' Nutrition Facts labels.
Foods high in soluble fiber also are part of the TLC diet. They help prevent the digestive tract from absorbing cholesterol. These foods include:
- Whole-grain cereals such as oatmeal and oat bran
- Fruits such as apples, bananas, oranges, pears, and prunes
- Legumes such as kidney beans, lentils, chick peas, black-eyed peas, and lima beans
A diet rich in fruits and vegetables can increase important cholesterol-lowering compounds in your diet. These compounds, called plant stanols or sterols, work like soluble fiber.
A healthy diet also includes some types of fish, such as salmon, tuna (canned or fresh), and mackerel. These fish are a good source of omega-3 fatty acids. These acids may help protect the heart from blood clots and inflammation and reduce the risk of heart attack. Try to have about two fish meals every week.
You also should try to limit the amount of sodium (salt) that you eat. This means choosing low-salt and "no added salt" foods and seasonings at the table or while cooking. The Nutrition Facts label on food packaging shows the amount of sodium in the item.
Try to limit drinks with alcohol. Too much alcohol will raise your blood pressure and triglyceride level. (Triglycerides are a type of fat found in the blood.) Alcohol also adds extra calories, which will cause weight gain.
Men should have no more than two drinks containing alcohol a day. Women should have no more than one drink containing alcohol a day. One drink is a glass of wine, beer, or a small amount of hard liquor.
For more information about TLC, go to the National Heart, Lung, and Blood Institute’s (NHLBI’s) "Your Guide to Lowering Your Cholesterol With TLC."
Weight Management
If you’re overweight or obese, losing weight can help lower LDL cholesterol. Maintaining a healthy weight is especially important if you have a condition called metabolic syndrome.
Metabolic syndrome is the name for a group of risk factors that raise your risk for heart disease and other health problems, such as diabetes and stroke.
The five metabolic risk factors are a large waistline (abdominal obesity), a high triglyceride level, a low HDL cholesterol level, high blood pressure, and high blood sugar. Metabolic syndrome is diagnosed if you have at least three of these metabolic risk factors.
Physical Activity
Routine physical activity can lower LDL cholesterol and triglycerides and raise your HDL cholesterol level.
People gain health benefits from as little as 60 minutes of moderate-intensity aerobic activity per week. The more active you are, the more you will benefit.
For more information about physical activity, go to the U.S. Department of Health and Human Services' "2008 Physical Activity Guidelines for Americans," the Health Topics Physical Activity and Your Heart article, and the NHLBI's "Your Guide to Physical Activity and Your Heart."
Cholesterol-Lowering Medicines
In addition to lifestyle changes, your doctor may prescribe medicines to help lower your cholesterol. Even with medicines, you should continue the TLC program.
Medicines can help control high blood cholesterol, but they don’t cure it. Thus, you must continue taking your medicine to keep your cholesterol level in the recommended range.
The five major types of cholesterol-lowering medicines are statins, bile acid sequestrants (seh-KWES-trants), nicotinic (nick-o-TIN-ick) acid, fibrates, and ezetimibe.
- Statins work well at lowering LDL cholesterol. These medicines are safe for most people. Rare side effects include muscle and liver problems.
- Bile acid sequestrants also help lower LDL cholesterol. These medicines usually aren’t prescribed as the only medicine to lower cholesterol. Sometimes they’re prescribed with statins.
- Nicotinic acid lowers LDL cholesterol and triglycerides and raises HDL cholesterol. You should only use this type of medicine with a doctor’s supervision.
- Fibrates lower triglycerides, and they may raise HDL cholesterol. When used with statins, fibrates may increase the risk of muscle problems.
- Ezetimibe lowers LDL cholesterol. This medicine works by blocking the intestine from absorbing cholesterol.
While you’re being treated for high blood cholesterol, you’ll need ongoing care. Your doctor will want to make sure your cholesterol levels are controlled. He or she also will want to check for other health problems.
If needed, your doctor may prescribe medicines for other health problems. Take all medicines exactly as your doctor prescribes. The combination of medicines may lower your risk for heart disease and heart attack.
While trying to manage your cholesterol, take steps to manage other heart disease risk factors too. For example, if you have high blood pressure, work with your doctor to lower it.
If you smoke, quit. Talk with your doctor about programs and products that can help you quit smoking. Also, try to avoid secondhand smoke. If you’re overweight or obese, try to lose weight. Your doctor can help you create a reasonable weight-loss plan.
Clinical Trials
The National Heart, Lung, and Blood Institute (NHLBI) is strongly committed to supporting research aimed at preventing and treating heart, lung, and blood diseases and conditions and sleep disorders.
NHLBI-supported research has led to many advances in medical knowledge and care. Often, these advances depend on the willingness of volunteers to take part in clinical trials.
Clinical trials test new ways to prevent, diagnose, or treat various diseases and conditions. For example, new treatments for a disease or condition (such as medicines, medical devices, surgeries, or procedures) are tested in volunteers who have the illness. Testing shows whether a treatment is safe and effective in humans before it is made available for widespread use.
By taking part in a clinical trial, you can gain access to new treatments before they’re widely available. You also will have the support of a team of health care providers, who will likely monitor your health closely. Even if you don’t directly benefit from the results of a clinical trial, the information gathered can help others and add to scientific knowledge.
If you volunteer for a clinical trial, the research will be explained to you in detail. You’ll learn about treatments and tests you may receive, and the benefits and risks they may pose. You’ll also be given a chance to ask questions about the research. This process is called informed consent.
If you agree to take part in the trial, you’ll be asked to sign an informed consent form. This form is not a contract. You have the right to withdraw from a study at any time, for any reason. Also, you have the right to learn about new risks or findings that emerge during the trial.
For more information about clinical trials related to high blood cholesterol, talk with your doctor. You also can visit the following Web sites to learn more about clinical research and to search for clinical trials:
- http://clinicalresearch.nih.gov
- www.clinicaltrials.gov
- www.nhlbi.nih.gov/studies/index.htm
- www.researchmatch.org
For more information about clinical trials for children, visit the NHLBI’s Children and Clinical Studies Web page.
Links to Other Information About High Blood Cholesterol
NHLBI Resources
- Aim for a Healthy Weight
- "Aim for a Healthy Weight" Patient Booklet
- Atherosclerosis (Health Topics)
- Cardiovascular Information for the Public
- Coronary Heart Disease (Health Topics)
- Coronary Heart Disease Risk Factors (Health Topics)
- "High Blood Cholesterol—What You Need to Know"
- Keep the Beat™ Deliciously Healthy Eating
- Physical Activity and Your Heart (Health Topics)
- Smoking and Your Heart (Health Topics)
- Story of Success: High Blood Cholesterol
- The 10-Year Heart Attack Risk Assessment Tool
- "Your Guide to a Healthy Heart"
- "Your Guide to Lowering Your Cholesterol With TLC"
- "Your Guide to Physical Activity and Your Heart"
Non-NHLBI Resources
- Cholesterol (MedlinePlus)
- Managing Cholesterol Interactive Tutorial (MedlinePlus—Patient Education Institute)
Clinical Trials
- Children and Clinical Studies
- Clinical Trials (Health Topics)
- Current Research (ClinicalTrials.gov)
- NHLBI Clinical Trials
- NIH Clinical Research Trials and You (National Institutes of Health)
- ResearchMatch (funded by the National Institutes of Health)
____________
™ Keep the Beat is a trademark of the U.S. Department of Health and Human Services.