Contraception
In the United States, almost half of all pregnancies are unintended.1 Yet, several safe and highly effective methods of contraception (birth control) are available to prevent unintended pregnancy. Since 2000, several new methods of birth control have become available in the United States, including the levonorgestrel-releasing intrauterine system, the hormonal contraceptive patch, the hormonal contraceptive ring, the hormonal implant, a 91-day regimen of oral contraceptives, two new barrier methods, and a new form of female sterilization. Learn more about the types of birth control available.
Most women of reproductive age in the United States use birth control. Between 2006–2008, 99% of women who had ever had sexual intercourse had used at least one method of birth control; however, 7.3% of women who were currently at risk of unintended pregnancy were not using a contraceptive method.2 The most popular method of birth control was the oral contraceptive pill, used by 10.7 million women in the United States, followed by female sterilization, condoms, male sterilization, and other methods of birth control.2 Approximately 10% of women had ever used emergency contraception.2
- Finer LB, Zolna MR. Unintended pregnancy in the United States: incidence and disparities, 2006 [PDF - 182KB] Contraception. 2011;84(5):478–485.
- Mosher WD, Jones J. Use of Contraception in the United States, 1982–2008 [PDF - 1.42MB] National Center for Health Statistics. National Vital Health Stat. 2010;23(29).
Types of Birth Control
The effectiveness of birth control methods is critically important for reducing the risk of unintended pregnancy. Intrauterine contraception and the contraceptive implant remain effective for years once correctly in place. The effectiveness of hormonal, barrier, and fertility awareness-based methods depends on correct and consistent use. For each of these methods, a range of effectiveness estimates is provided; lower estimates are based on typical use and higher estimates are based on perfect use.
Intrauterine Contraception
- Copper T intrauterine device (IUD) —An IUD is a small device that is shaped in the form of a “T.” Your doctor places it inside the uterus to prevent pregnancy. It can stay in your uterus for up to 10 years. This IUD is more than 99% effective at preventing pregnancy.
- Levonorgestrel intrauterine system (IUS)—The IUS is a small T-shaped device like the IUD. It is placed inside the uterus by a doctor. It releases a small amount of progestin each day to keep you from getting pregnant. The IUS stays in your uterus for up to 5 years. The IUS is more than 99% effective at preventing pregnancy.
Hormonal Methods
- Implant—The implant is a single, thin rod that is inserted under the skin of a women’s upper arm. The rod contains a progestin that is released into the body over 3 years. It is 99% effective at preventing pregnancy.
- Injection or "shot"— Women get shots of the hormone progestin in the buttocks or arm every three months from their doctor. It is 94–99% effective at preventing pregnancy.
 Combined oral contraceptives—Also called “the pill,”combined oral contraceptives contain the hormones estrogen and progestin. It is prescribed by a doctor. A pill is taken at the same time each day. If you are older than 35 years and smoke, have a history of blood clots or breast cancer, your doctor may advise you not to take the pill. The pill is 91–99% effective at preventing pregnancy.
Combined oral contraceptives—Also called “the pill,”combined oral contraceptives contain the hormones estrogen and progestin. It is prescribed by a doctor. A pill is taken at the same time each day. If you are older than 35 years and smoke, have a history of blood clots or breast cancer, your doctor may advise you not to take the pill. The pill is 91–99% effective at preventing pregnancy.- Progestin only pill—Unlike the combined pill, the progestin-only pill (sometimes called the mini-pill) only has one hormone, progestin, instead of both estrogen and progestin. It is prescribed by a doctor. It is taken at the same time each day. It is a good option for women who can’t take estrogen. They are 91–99% effective at preventing pregnancy.
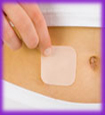 Patch—This skin patch is worn on the lower abdomen, buttocks, or upper body (but not on the breasts). This method is prescribed by a doctor. It releases hormones progestin and estrogen into the bloodstream. You put on a new patch once a week for three weeks. During the fourth week, you do not wear a patch, so you can have a menstrual period. The patch is 91–99% effective at preventing pregnancy, but it appears to be less effective in women who weigh more than 198 pounds.
Patch—This skin patch is worn on the lower abdomen, buttocks, or upper body (but not on the breasts). This method is prescribed by a doctor. It releases hormones progestin and estrogen into the bloodstream. You put on a new patch once a week for three weeks. During the fourth week, you do not wear a patch, so you can have a menstrual period. The patch is 91–99% effective at preventing pregnancy, but it appears to be less effective in women who weigh more than 198 pounds. - Hormonal vaginal contraceptive ring— The ring releases the hormones progestin and estrogen. You place the ring inside your vagina. You wear the ring for three weeks, take it out for the week you have your period, and then put in a new ring. It is 91–99% effective at preventing pregnancy.
- Emergency contraception—Emergency contraception is NOT a regular method of birth control. Emergency contraception can be used after no birth control was used during sex, or if the birth control method failed, such as if a condom broke.
- Women can take emergency contraceptive pills up to 5 days after unprotected sex, but the sooner the pills are taken, the better they will work. There are three different types of emergency contraceptive pills available in the United States. Some emergency contraceptive pills are available over the counter for women 17 years of age or older. If younger than 17 years, emergency contraceptive pills are available by prescription.
- Another type of emergency contraception is having your doctor insert the Copper T IUD into your uterus within seven days of unprotected sex. This method is 99% effective at preventing pregnancy.
Barrier Methods
- Male condom—Worn by the man, a male condom keeps sperm from getting into a woman’s body. Latex condoms, the most common type, help prevent pregnancy and HIV and other STDs as do the newer synthetic condoms. “Natural” or “lambskin” condoms also help prevent pregnancy, but may not provide protection against STDs, including HIV. Male condoms are 82–98% effective at preventing pregnancy. Condoms can only be used once. You can buy condoms, KY jelly, or water-based lubricants at a drug store. Do not use oil-based lubricants such as massage oils, baby oil, lotions, or petroleum jelly with latex condoms. They will weaken the condom, causing it to tear or break.
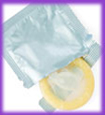
- Female condom—Worn by the woman, the female condom helps keeps sperm from getting into her body. It is packaged with a lubricant and is available at drug stores. It can be inserted up to eight hours before sexual intercourse. Female condoms are 79–95% effective at preventing pregnancy, and also may help prevent STDs.
- Diaphragm or cervical cap—Each of these barrier methods are placed inside the vagina to cover the cervix to block sperm. The diaphragm is shaped like a shallow cup. The cervical cap is a thimble-shaped cup.Before sexual intercourse, you insert them with spermicide to block or kill sperm.
 The diaphragm is 84–94% effective at preventing pregnancy. Visit your doctor for a proper fitting because diaphragms and cervical caps come in different sizes.
The diaphragm is 84–94% effective at preventing pregnancy. Visit your doctor for a proper fitting because diaphragms and cervical caps come in different sizes. - Spermicides—These products work by killing sperm and come in several forms—foam, gel, cream, film, suppository, or tablet. They are placed in the vagina no more than one hour before intercourse. You leave them in place at least six to eight hours after intercourse. You can use a spermicide in addition to a male condom, diaphragm, or cervical cap. Spermicides alone are about 72–82% effective at preventing pregnancy. They can be purchased at drug stores.

Fertility Awareness-Based Methods
- Natural family planning or fertility awareness—Understanding your monthly fertility pattern can help you plan to get pregnant or avoid getting pregnant. Your fertility pattern is the number of days in the month when you are fertile (able to get pregnant), days when you are infertile, and days when fertility is unlikely, but possible. If you have a regular menstrual cycle, you have about nine or more fertile days each month. If you do not want to get pregnant, you do not have sex on the days you are fertile, or you use a barrier method of birth control on those days. These fertility awareness-based methods are 75–96% effective at preventing pregnancy.
Contraceptive sterilization is a permanent, safe, and highly effective approach for birth control. These methods are meant for people who are sure that they do not desire a pregnancy in the future.
The following methods are more than 99% effective at preventing pregnancy.
- Female Sterilization—Tubal ligation or “tying tubes”— A woman can have her fallopian tubes tied (or closed) so that sperm and eggs cannot meet for fertilization. The procedure can be done in a hospital or in an outpatient surgical center. You can go home the same day of the surgery and resume your normal activities within a few days. This method is effective immediately.
- Transcervical Sterilization— A thin tube is used to thread a tiny device into each fallopian tube. It irritates the fallopian tubes and causes scar tissue to grow and permanently plug the tubes. It can take about three months for the scar tissue to grow, so use another form of birth control during this time. Return to your doctor for a test to see if scar tissue has fully blocked your fallopian tubes.
- Male Sterilization–Vasectomy—This operation is done to keep a man’s sperm from going to his penis, so his ejaculate never has any sperm in it that can fertilize an egg. The procedure is done at an outpatient surgical center. The man can go home the same day. Recovery time is less than one week. After the operation, a man visits his doctor for tests to count his sperm and to make sure the sperm count has dropped to zero; this takes about 12 weeks. Another form of birth control should be used until the man’s sperm count has dropped to zero.
Although most women and men who undergo contraceptive sterilization do not regret having had the procedure, the permanence of the method is an important consideration, as regret has been documented in studies. For example, the U.S. Collaborative Review of Sterilization (CREST) study found that women who were younger at the time of the procedure were more likely to experience regret. Read the following to learn more:
- Poststerilization regret: findings from the United States Collaborative Review of Sterilization. Obstet Gynecol. 1999;93:889–895.
- Regret following female sterilization at a young age: a systematic review. Contraception. 2006;73(2):205–210.
- Abstracts of publications from the Collaborative Review of Sterilization (CREST) study. [PDF - 153]
An additional issue addressed by the CREST study was the question of whether women who underwent contraceptive sterilization developed a “post-tubal ligation syndrome” of menstrual abnormalities, something that had been debated for years. Results indicated that menstrual abnormalities were no more common among women who had undergone tubal sterilization than among women who had not. (The risk of menstrual abnormalities after tubal sterilization. [PDF - 98KB] N Engl J Med. 2000;343:1681–1687).
- The risk of pregnancy after vasectomy. Obstetrics and Gynecology. 2004;103:848–850.
- A comparison of women’s regret following vasectomy versus tubal sterilization. Obstetrics and Gynecology. 2002;99:1073–1079.
- Contraceptive sterilization among married adults: national data on who chooses vasectomy and tubal sterilization. Contraception. 2011 Nov 29. [Epub ahead of print] PMID: 22133657
When considering a vasectomy, it’s important to understand that failures can occur. CDC research has estimated there is a probability of 11 failures per 1,000 procedures over 2 years; half of the failures occurred in the first three months after the vasectomy, and no failures occurred after 72 weeks.1 CDC research also examined regret among women whose partner underwent a vasectomy.2 In interviews with female partners of men who received vasectomies, CDC found that while most women did not regret their husband's vasectomies, the probability of regret over 5 years was about 6%. This is why it is important to know facts about this and other permanent forms of birth control before making a decision.
Resources for Consumers
- Birth Control Methods fact sheet (women'shealth.gov)
Métodos anticonceptivos hoja de datos - Emergency Contraception (emergency birth control) fact sheet (women'shealth.gov)
Anticoncepción de emergencia hoja de datos - Office of Population Affairs Find a Title-X family planning provider
- Birth Control (FDA)
- Planned Parenthood
Resources for Providers
- U S. Medical Eligibility Criteria for Contraceptive Use CDC went through a formal adaptation process to create the United States Medical Eligibility Criteria for Contraceptive Use (USMEC). This guidance is intended to assist health care providers when counseling women, men, and couples about contraceptive method choice.
- Contraceptive Methods Available to Patients of Office-Based Physicians and Title X Clinics—United States, 2009–2010
CDC researchers conducted a survey to determine the availability of specific types of contraceptives in offices serving women of reproductive age. Results indicate a higher proportion of Title X clinic providers than office-based physicians offered a range of contraceptive methods on-site, but availability of long-acting, reversible contraceptives (LARCs), including IUDs and contraceptive implants, often depended on referral to other providers. Improving contraceptive delivery by increasing on-site availability in physicians' offices and clinics of a range of contraceptive methods, including LARCs, might increase contraceptive use and reduce rates of unintended pregnancy.
Source: MMWR. 2011;60(01):1–4. - Contraceptive Use Among Postpartum Women—12 States and New York City, 2004–2006 CDC researchers analyzed PRAMS data that included more than 43,000 postpartum women in 12 states and New York City and found that only 62% reported using effective contraceptive methods with failure rates of less than 10% under typical use (hormonal methods, male or female sterilization, or intrauterine devices (IUDs)). Source: MMWR. 2009;58(30):821–826.
- Postpartum intrauterine device insertion and postpartum tubal sterilization in the United States Among U.S. postpartum women, IUD insertion occurs considerably less frequently than tubal sterilization, even among younger women for whom poststerilization regret is a concern. American Journal of Obstetrics & Gynecology. 2011 Aug 11. [Epub ahead of print]
- Contraceptive sterilization among married adults: national data on who chooses vasectomy and tubal sterilization Vasectomy and tubal sterilization tend to be used by different segments of the married population as characterized by education, income, and other factors. To be effective, efforts to promote vasectomy use need to understand the reasons behind these differences. Increasing the availability and use of vasectomy will require education about its benefits. Contraception. 2011 Nov 29. [Epub ahead of print]
- American Congress of Obstetricians and Gynecology
- Data and Statistics—Unintended Pregnancy
Contact Us:
- Centers for Disease Control and Prevention
1600 Clifton Rd
Atlanta, GA 30333 - 800-CDC-INFO
(800-232-4636)
TTY: (888) 232-6348 - New Hours of Operation
8am-8pm ET/Monday-Friday
Closed Holidays - cdcinfo@cdc.gov


