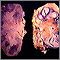
Disseminated tuberculosis
Disseminated tuberculosis (TB) is a contagious bacterial infection that has spread from the lungs to other parts of the body through the blood or lymph system.
See also: Tuberculosis - pulmonary
Causes
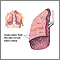
Tuberculosis (TB) infection can develop after inhaling droplets sprayed into the air from a cough or sneeze by someone infected with the Mycobacterium tuberculosis bacteria. Small areas of infection, called granulomas (granular tumors), develop in the lungs.
The usual site of TB is the lungs, but other organs can be involved. In the U.S., most people with primary tuberculous get better and have no further evidence of disease. Disseminated TB develops in the small number of infected people whose immune systems do not successfully contain the primary infection.
Disseminated disease can occur within weeks of the primary infection. Sometimes, it does not occur until years after you become infected. You are more likely to get this type of TB if you have a weaken immune system due to disease (such as AIDS) or certain medications. Infants and the elderly are also at higher risk.
Your risk for catching TB increases if you:
- Are around people who have the disease
- Live in crowded or unclean conditions
- Have poor nutrition
TB has become more common in the U.S. in recent years. This may be due to a larger number of TB infections in people with AIDS and HIV, an increase in the number of immune-suppressing medications, and increasing numbers of homeless people. A rise in drug-resistant strains of TB bacteria also plays a role.
Symptoms
Disseminated tuberculosis can affect many different body areas. Symptoms can include:
- Cough
- Fatigue
- Fever
- General discomfort, uneasiness, or ill feeling (malaise)
- Shortness of breath
- Sweating
- Weight loss
Other symptoms that can occur with this disease:
- Abdominal swelling
- Chills
- Joint pain
- Pale skin due to anemia (pallor)
- Swollen glands
Note: The symptoms will depend upon the affected areas of the body.
Exams and Tests
A physical exam may show:
Tests for TB include:
- Biopsies and cultures of affected organs or tissues
- Bronchoscopy for biopsy or culture
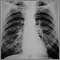
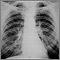
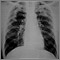
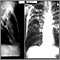
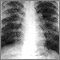
- Chest x-ray
- CT scan of the affected area
- Fundoscopy may reveal retinal lesions
- Lung biopsy
- Mycobacterial culture of bone marrow or blood
- Pleural biopsy
- Sputum cultures
- Tuberculin skin test
This list may not be all-inclusive.
The disease may also alter the results of the following tests:
- Complete blood count (CBC)
- Peripheral blood smear
- Blood calcium level
Treatment
The goal of treatment is to cure the infection with drugs that fight the TB bacteria. Treatment of active pulmonary TB will always involve a combination of many drugs (usually four drugs). All of the drugs are continued until lab tests show which medicines work best.
The most commonly used drugs include:
- Isoniazid
- Rifampin
- Pyrazinamide
- Ethambutol
Other drugs that may be used to treat TB include:
- Amikacin
- Ethionamide
- Moxifloxacin
- Para-aminosalicylic acid
- Streptomycin
You may need to take many different pills at different times of the day for 6 months or longer. It is very important that you take the pills the way your health care provider instructed.
When people do not take their tuberculosis medications as recommended, the infection becomes much more difficult to treat. The TB bacteria may become resistant to treatment, and sometimes, the drugs no longer help treat the infection.
When there is a concern that a patient may not take all the medication as directed, a health care provider may need to watch the person take the prescribed drugs. This is called directly observed therapy. In this case, drugs may be given 2 or 3 times per week, as prescribed by a doctor.
You may need to stay at home or be admitted to a hospital for 2 - 4 weeks to avoid spreading the disease to others until you are no longer contagious.
Your doctor or nurse is required by law to report your TB illness to the local health department. Your health care team will be sure that you receive the best care for your TB.
Outlook (Prognosis)
Most forms of disseminated TB respond well to treatment.
Possible Complications
Complications of disseminated TB can include:
- Adult respiratory distress syndrome (ARDS)
- Liver inflammation
- Lung failure
- Relapse of the disease
Medicines used to treat TB may cause side effects, including liver problems. Other side effects include:
- Changes in vision
- Orange- or brown-colored tears and urine
- Rash
A vision test may be done before treatment so your doctor can monitor any changes in your eyes' health over time.
When to Contact a Medical Professional
Call your health care provider if you know or suspect that you have been exposed to TB. All forms of TB and exposure need prompt evaluation and treatment.
Prevention
TB is a preventable disease, even in those who have been exposed to an infected person. Skin testing for TB is used in high risk populations or in people who may have been exposed to TB, such as health care workers.
A positive skin test in a person without symptoms is a sign of TB exposure. Discuss preventive therapy with your doctor. People who have been exposed to TB should be skin tested immediately and have a follow-up test at a later date, if the first test is negative.
Prompt treatment is extremely important in controlling the spread of TB from those who have active TB disease to those who have never been infected with TB.
Some countries with a high incidence of TB give people a vaccination (called BCG) to prevent TB. However, the effectiveness of this vaccine is controversial and it is not routinely used in the United States.
People who have had BCG may still be skin tested for TB. Discuss the test results (if positive) with your doctor.
Alternative Names
Miliary tuberculosis; Tuberculosis - disseminated; Extrapulmonary tuberculosis
References
Ellner JJ. Tuberculosis. In: Goldman L, Schafer AI, eds.Cecil Medicine. 24th ed.Philadelphia,PA: Saunders Elsevier; 2011:chap 332.
Fitzgerald DW, Sterling TR, Haas DW. Mycobacterium tuberculosis. In: Mandell GL, Bennett JE, Dolan R, eds. Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. 7th ed. Orlando, FL: Saunders Elsevier; 2009:chap 250.
Update Date: 12/6/2011
Updated by: David C. Dugdale, III, MD, Professor of Medicine, Division of General Medicine, Department of Medicine, University of Washington School of Medicine; Jatin M. Vyas, MD, PhD, Assistant Professor in Medicine, Harvard Medical School, Assistant in Medicine, Division of Infectious Disease, Department of Medicine, Massachusetts General Hospital. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.
MedlinePlus Topics
Images
Read More

A.D.A.M., Inc. is accredited by URAC, also known as the American Accreditation HealthCare Commission (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics and subscribes to the principles of the Health on the Net Foundation (www.hon.ch).
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 1997-2012, A.D.A.M., Inc. Duplication for commercial use must be authorized in writing by ADAM Health Solutions.