Cervicitis
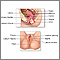
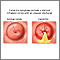
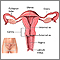
Cervicitis is swelling (inflammation) of the end of the uterus (cervix).
Causes
Cervicitis is most often caused by an infection, usually caught during sexual activity. Sexually transmitted infections (STIs) that can cause cervicitis include:
- Chlamydia
- Gonorrhea
- Herpes virus (genital herpes)
- Human papilloma virus (genital warts)
- Trichomoniasis
Cervicitis may sometimes be caused by:
- A device inserted into the pelvic area such as:
- Cervical cap
- Device to support the uterus (pessary)
- Diaphragm
- Allergy to spermicides used for birth control
- Allery to latex in condoms
- Exposure to a chemical
Cervicitis is very common, affecting more than half of all women at some point during their adult life. Risks include:
- High-risk sexual behavior
- History of STIs
- Many sexual partners
- Sex (intercourse) at an early age
- Sexual partners who have engaged in high-risk sexual behavior or have had an STI
Bacteria (such as staphylococcus and streptococcus) and too much growth of normal bacteria in the vagina (bacterial vaginosis) can also cause cervicitis.
Symptoms
- Abnormal vaginal bleeding
- After intercourse
- After menopause
- Between periods
- Unusual vaginal discharge
- Does not go away
- Gray, white, or yellow color
- May have an odor
- Painful sexual intercourse
- Pain in the vagina
- Pressure or heaviness in the pelvis
Note: There may be no symptoms, so it is recommended that certain women be tested for chlamydia, even if they do not have symptoms.
Exams and Tests
A pelvic examination may show:
- Discharge from the cervix
- Redness of the cervix
- Swelling (inflammation) of the walls of the vagina
Tests:
- Inspection of the discharge under a microscope (may show candidiasis, trichomoniasis, or bacterial vaginosis)
- Pap smear
- Tests for gonorrhea or chlamydia
Rarely, colposcopy and biopsy of the cervix is necessary.
Treatment
Antibiotics are used to treat bacterial infections, such as chlamydia, gonorrhea, and others. Drugs called antivirals may be used to treat herpes infections.
Hormonal therapy (with estrogen or progesterone) may be used in women who have reached menopause (postmenopausal).
When these treatments have not worked or when cervicitis has been present for a long time, treatment may include:
- Cryosurgery (freezing)
- Electrocauterization
- Laser therapy
Outlook (Prognosis)
Simple cervicitis usually heals with treatment if the cause is found and there is a treatment for that cause.
Cervicitis can last for months or years.
Possible Complications
Cervicitis may last for months to years. Cervicitis may lead to pain with intercourse (dyspareunia).
When to Contact a Medical Professional
Call your health care provider if you have symptoms of cervicitis.
Prevention
Here are some ways to reduce your risk of cervicitis:
- Avoid chemical irritants such as douches and deodorant tampons.
- Make sure that any foreign objects you insert into your vagina (such as tampons) are placed properly. Be sure to follow instructions on how long to leave it inside, how often to change it, or how often to clean it.
- Not having sexual intercourse (abstinence) is the only absolute method of preventing sexually transmitted cervicitis. A monogamous sexual relationship with someone who is known to be free of any STI can reduce the risk. Monogamous means you and your partner do not have sex with any other people. See: Safe Sex
- You can greatly lower your risk of catching an STI by using a condom every time you have sex. Condoms are available for both men and women, but are most commonly worn by the man. A condom must be used properly every time.
See also:
Alternative Names
Cervical inflammation; Inflammation - cervix
References
Eckert LO, Lentz GM. Infections of the lower genital tract: Vulva, vagina, cervix, toxic shock syndrome, HIV infections. In: Katz VL, Lentz GM, Lobo RA, Gershenson DM, eds. Comprehensive Gynecology. 5th ed. Philadelphia, Pa: Mosby Elsevier; 2007:chap 2
Zeimet A, McBride DR, Basilan R, Roland WE, McCrary D, Hoonmo K. Infectious diseases. In: Rakel RE, ed. Textbook of Family Medicine. 8th ed. Philadelphia, Pa: Saunders Elsevier; 2011:chap 16.
Centers for Disease Control and Prevention. Sexually Transmitted Diseases Treatment Guidelines, 2010. MMWR 2010;59(No. RR-12)
Update Date: 2/26/2012
Updated by: Linda J. Vorvick, MD, Medical Director and Director of Didactic Curriculum, MEDEX Northwest Division of Physician Assistant Studies, Department of Family Medicine, UW Medicine, School of Medicine, University of Washington. Susan Storck, MD, FACOG, Chief, Eastside Department of Obstetrics and Gynecology, Group Health Cooperative of Puget Sound, Bellevue, Washington; Clinical Teaching Faculty, Department of Obstetrics and Gynecology, University of Washington School of Medicine. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.

A.D.A.M., Inc. is accredited by URAC, also known as the American Accreditation HealthCare Commission (www.urac.org). URAC's accreditation program is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s editorial policy, editorial process and privacy policy. A.D.A.M. is also a founding member of Hi-Ethics and subscribes to the principles of the Health on the Net Foundation (www.hon.ch).
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 1997-2012, A.D.A.M., Inc. Duplication for commercial use must be authorized in writing by ADAM Health Solutions.