Inside this Chapter
- RECOMMENDATIONS HIGHLIGHTS
- 10.1 THE PROMISE OF HEALTH IT AND THE ROLE OF BROADBAND
- 10.2 THE NEED FOR ACTION: MAXIMIZING HEALTH IT UTILIZATION
- 10.3 CLOSING THE BROABAND-ENABLED HEALTH IT ADOPTION GAP
- 10.4 UNLOCKING THE VALUE OF DATA
- 10.5 CLOSING THE HEALTH IT BROADBAND CONNECTIVITY GAP
Improving Americans’ health is one of the most important tasks for the nation. Health care already accounts for 17% of U.S. gross domestic product (GDP); by 2020, it will top 20% .1 America is aging— by 2040, there will be twice as many Americans older than 65 as there are today—and health care costs will likely increase as a consequence.
Rising costs would be less concerning if there were results. But Americans are not healthy. Sixty-one percent of American adults are overweight or obese, which often leads to medical complications.2 Chronic conditions, which already account for 75%3 of the nation’s health care costs, are increasing across all ages.4 The nation has 670,000 new cases of congestive heart failure every year, many of them fatal.5 And too often the care itself causes harm. One and a half million Americans are injured every year because of prescription drug errors,6 while a person dies every six minutesfrom an infection developed after arriving at a hospital.7
In addition, the United States has a health care supply problem. The country is expected to have a shortage of tens of thousands of physicians by 2020.8 An aging physician workforce that is nearing retirement and working fewer hours exacerbates the situation.9 Supply will be further strained if previously uninsured Americans enter the care delivery system.
Another significant problem plaguing the nation’s health care system is the fact that there are health disparities across different ethnic groups. “African Americans, for example, experience the highest rates of mortality from heart disease, cancer, cerebrovascular disease, and HIV/AIDS than any other U.S. racial or ethnic group. Hispanic Americans are almost twice as likely as non-Hispanic whites to die from diabetes. Some Asian Americans experience rates of stomach, liver and cervical cancers that are well above national averages.”10 Further exacerbating this problem, members of ethnic groups are less likely than whites to have health insurance, have more difficulty getting health care and have fewer choices in where to receive care.11
Broadband is not a panacea. However, there is a developing set of broadband-enabled solutions that can play an important role in the transformation required to address these issues. These solutions, usually grouped under the name health information technology, offer the potential to improve health care outcomes while simultaneously controlling costs and extending the reach of the limited pool of health care professionals. Furthermore, as a major area of innovation and entrepreneurial activity, the health IT industry can serve as an engine for job creation and global competitiveness.
This chapter’s recommendations aim to encourage maximum utilization of these solutions. In its traditional role, the FCC would evaluate this challenge primarily through a network connectivity perspective. However, it is the ecosystem of networks, applications, devices and individual actions that drives value, not just the network itself. It is imperative to focus on adoption challenges, and specifically the government decisions that influence the system in which private actors operate, if America is to realize the enormous potential of broadband-enabled health IT.
This chapter has five sections. Section 10.1 reviews the potential value that broadband-enabled health IT solutions can unlock. Section 10.2 offers an overview of current health IT utilization in America, reviews recent federal government actions to enhance utilization of health IT and highlights outstanding challenges.
Sections 10.3-10.5 provide recommendations concerning four critical areas in which the government should take action to help unlock the value of broadband and health IT: better reimbursement, modern regulation, increased data capture and utilization and sufficient connectivity.
RECOMMENDATIONS
Create appropriate incentives for e-care utilization.
Modernize regulation to enable health IT adoption.
- Congress, states and the Centers for Medicare & Medicaid Services (CMS) should consider reducing regulatory barriers that inhibit adoption of health IT solutions.
- The FCC and the Food and Drug Administration (FDA) should clarify regulatory requirements and the approval process for converged communications and health care devices.
Unlock the value of data.
- The Office of the National Coordinator for Health Information Technology (ONC) should establish common standards and protocols for sharing administrative, research and clinical data, and provide incentives for their use.
- Congress should consider providing consumers access to—and control over—all their digital health care data in machine-readable formats in a timely manner and at a reasonable cost.
Ensure sufficient connectivity for health care delivery locations.
- The FCC should replace the existing Internet Access Fund with a Health Care Broadband Access Fund.
- The FCC should establish a Health Care Broadband Infrastructure Fund to subsidize network deployment to health care delivery locations where existing networks are insufficient.
- The FCC should authorize participation in the Health Care Broadband Funds by long-term care facilities, off-site administrative offices, data centers and other similar locations. Congress should consider providing support for for-profit institutions that serve particularly vulnerable populations.
- To protect against waste, fraud and abuse in the Rural Health Care Program, the FCC should require participating institutions to meet outcomes-based performance measures to qualify for Universal Service Fund (USF) subsidies, such as HHS’s meaningful use criteria.
- Congress should consider authorizing an incremental sum (up to $29 million per year) for the Indian Health Service (IHS) for the purpose of upgrading its broadband service to meet connectivity requirements.
- The FCC should periodically publish a Health Care Broadband Status Report.
10.1 THE PROMISE OF HEALTH IT AND THE ROLE OF BROADBAND
Health IT plays a key role in advancing policy priorities that improve health and health care delivery. Priorities set forth by HHS include the following:12
- Improving care quality, safety, efficiency and reducing disparities
- Engaging patients and families in managing their health
- Enhancing care coordination
- Improving population and public health
- Ensuring adequate privacy and security of health information
Health IT supports these priorities by dramatically improving the collection, presentation and exchange of health care information, and by providing clinicians and consumers the tools to transform care. Technology alone cannot heal, but when appropriately incorporated into care, technology can help health care professionals and consumers make better decisions, become more efficient, engage in innovation, and understand both individual and public health more effectively.
Analysis of information gathered through health IT can provide a basis for payment reform. Payors, providers and patients are focusing increasingly on value. However, data to measure the effectiveness of prevention and treatment on individual and population-wide bases are lacking. This hampers attempts to shift from a volume-focused system that pays for visits and procedures to a value-based regime that rewards cost-effective health improvements.14
Broadband is necessary for these transformations in three ways. First, it enables efficient exchange of patient and treatment information by allowing providers to access patients’ electronic health records (EHRs) from on-site or hosted locations. Second, it removes geography and time as barriers to care by enabling video consultation and remote patient monitoring. Third, broadband provides the foundation for the next generation of health innovation and connected-care solutions.
Box 10-1: Explanation of Referenced Terms13

Broadband and Electronic Health Records
Physicians report that electronic health records improve patient care in many ways.15 The e-prescribing component of EHRs helps avert known drug allergic reactions and potentially dangerous drug interactions, while facilitating the ordering of laboratory tests and reducing redundancy and errors. EHRs also provide easier access to critical laboratory information and enhance preventive care. For example, influenza and pneumonia vaccination reminders displayed to clinicians during a patient visit could play a part in saving up to 39,000 lives a year.16
According to one study often cited, electronic health record systems have the potential to generate net savings of $371 billion for hospitals and $142 billion for physician practices from safety and efficiency gains over 15 years.17 Potential savings from preventing disease and better managing chronic conditions could double these estimates.18
Hosted EHR solutions tend to be more affordable and easier-to-manage alternatives for small physician practices and clinics. In certain settings, they cost on average 20% less than on-site solutions, reduce the need for internal IT expertise and provide timely updates to clinical decision-support tools (e.g., drug interaction references and recommended care guidelines).19
Broadband and Video Consultation
Video consultation is especially beneficial for extending the reach of under-staffed specialties to patients residing in rural areas, Tribal lands and health professional shortage areas (HPSAs).20 For example, the American Heart Association and American Stroke Association recommend use of video consultation technology for stroke patients to help overcome the dearth of neurologists and to make decisions about whether to deliver the life-saving, clot-busting drug known as tPA (see Box 10-2).21
Box 10-2: Stroke Victim Makes Full Recovery—Thanks to E-Care22
At only 49 years of age, Beverly suffered a stroke. Her best friend drove her to St. Luke's Hospital, which has a video link to the stroke center at Massachusetts General Hospital (“Mass General”), 75 miles away. Minutes after her arrival, St. Luke’s emergency department staff assessed her symptoms, ordered a brain scan and called Mass General.
A Mass General stroke specialist activated a video link through which he could see Beverly on a gurney at St. Luke's. He had to determine whether she was having a stroke and, if so, what caused it. A hemorrhage could require emergency brain surgery, whereas a clot could be treated with tPA, which must be administered within the first three hours of stroke onset. The wrong diagnosis could prove fatal.
The specialist conducted a neurologic exam over the video link while receiving critical vital signs and lab values. He determined a clot was the cause and figured out when the stroke started by asking her yes/no questions to which she could nod her responses.
Beverly received tPA right at the three-hour deadline. An ambulance took her to Mass General and at the end of the hour-long ride, the nurse recalled being shocked at Beverly’s recovery—“We were literally pulling into Mass General, and I said, ‘Beverly, how are you?’ And she said, ‘I'm fine!’” It was as if all the symptoms were gone.
“Wow! I can talk!” the nurse remembers Beverly exclaiming. “'Wow, if it’s that medicine, it really worked!”
In addition to increasing access to otherwise unavailable care, video consultations combined with store-and-forward technologies (e.g., sending images to a specialist at night, as opposed to obtaining a diagnosis during a patient’s visit)23 could lead to significant cost savings from not having to transport patients. Avoiding costs from moving patients from correctional facilities and nursing homes to emergency departments and physician offices, or from one emergency department to another, could result in $1.2 billion in annual savings.24
Video consultation and remote access to patient data may also be critical during pandemic situations. If hospitals are at capacity or if isolation protocols are necessary to prevent the spread of infection, these technologies can help health care providers assist more patients and help patients avoid public areas.
Broadband and Remote Patient Monitoring
Remote patient monitoring enables early detection of health problems, usually before the onset of noticeable symptoms. Earlier detection allows earlier treatment and, therefore, better outcomes. For example, after an initial hospitalization for heart failure, 60% of patients are readmitted at least once within six to nine months.25 If a congestive heart failure patient has a common problem indicator, such as increase in weight or a change in fluid status, a monitoring system instantly alerts the clinician who can adjust medications, thereby averting a hospital readmission. Estimates indicate that remote monitoring could generate net savings of $197 billion over 25 years from just four chronic conditions.26
Box 10-3: How Health IT Saves Veterans Affairs Billions Each Year27
The Veterans Health Administration (VHA) coordinates the care of 32,000 veteran patients with chronic conditions through a national program called Care Coordination/Home Telehealth (CCHT). CCHT involves the systematic use of health informatics, e-care, and disease management technologies to avoid unnecessary admission to long-term institutional care. Technologies include videophones, messaging devices, biometric devices, digital cameras and remote monitoring devices.
CCHT led to a 25% reduction in the number of bed days of care and a 19% drop in hospital admissions. At $1,600 per patient per year, it costs far less than the VHA’s home-based primary care services ($13,121 per year) and nursing home care rates ($77,745 on average per patient per year).
Based on the VHA’s experience, e-care is an appropriate and cost-effective way to manage chronic care patients in urban and rural settings. Most importantly, it enables patients to live independently at home.
Mobile Broadband and the Future of Health
Mobile health is a new frontier in health innovation. This field encompasses applications, devices and communications networks that allow clinicians and patients to give and receive care anywhere at any time. Physicians download diagnostic data, lab results, images and drug information to handheld devices like PDAs and smartphones; emergency medical responders use field laptops to keep track of patient information and records; and patients use health monitoring devices and sensors that accompany them everywhere.28 Through capabilities like these, mobile health offers convenience critical to improving consumer engagement and clinician responsiveness.
Innovations in mobile medicine include new modalities of non-invasive sensors and body sensor networks.29 Mobile sensors in the form of disposable bandages and ingestible pills relay real-time health data (e.g., vital signs, glucose levels, and medication compliance) over wireless connections.30 Sensors that help older adults live independently at home detect motion, sense mood changes and help prevent falls.31 Wireless body sensor networks reduce infection risk and increase patient mobility by eliminating cables; they also improve caregiver effectiveness. Each of these solutions is available today, albeit with varying degrees of adoption.
Mobile medicine takes remote monitoring to a new level. For example, today’s mobile cardiovascular solutions allow a patient’s heart rhythm to be monitored continuously regardless of the patient’s whereabouts.32 Diabetics can receive continuous, flexible insulin delivery through real-time glucose monitoring sensors that transmit data to wearable insulin pumps.33
Advances in networked implantable devices enable capabilities that did not seem possible a few years ago. For example, micropower medical network services support wideband medical implant devices designed to restore sensation, mobility and other functions to paralyzed limbs and organs.34 These solutions offer great promise in improving the quality of life for numerous populations, including injured soldiers, stroke victims and those with spinal cord injuries. Human clinical trials of networked implantable devices targeting an array of conditions are expected to begin at the end of 2010.35
Mobile and networked health solutions are in their infancy. The applications and capabilities available even two years from now are expected to vary markedly from those available today. Some will be in specialized devices; others will be applications using capabilities already built into widely available mobile phones, such as global positioning systems and accelerometers. Networked implantable devices stand to grow in sophistication and broaden the realm of conditions they can address. These solutions represent a glimpse into the future of personal and public health—an expanded toolkit to achieve better health, quality of life and care delivery.
10.2 THE NEED FOR ACTION: MAXIMIZING HEALTH IT UTILIZATION
Limited Health IT Utilization
The United States is not taking full advantage of the opportunities that health IT provides. It lags other developed countries in health IT adoption among primary health care providers (see Exhibit 10-A).
Exhibit 10-A: International Comparison of Electronic Health Adoption 36
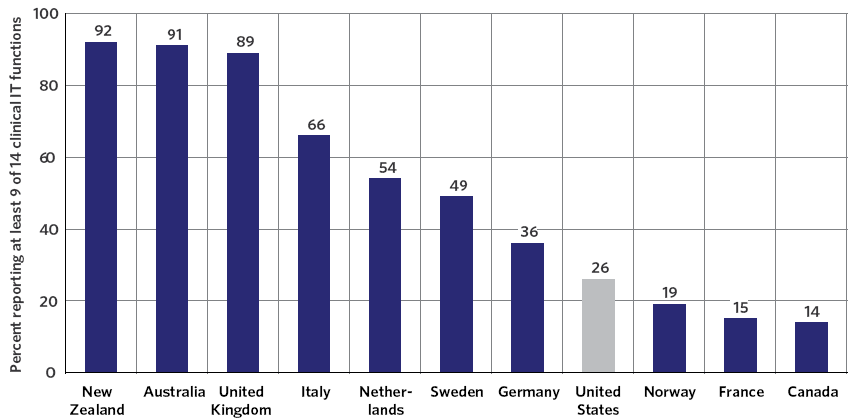
The United States ranks in the bottom half (out of 11 countries) on every metric used to measure adoption, including use of electronic medical records (10th), electronic prescribing (10th), electronic clinical note entry (10th), electronic ordering of laboratory tests (8th), electronic alerts/prompts about potential drug dose/interaction problems (8th) and electronic access to patient test results (7th).
Adoption rates for e-care are similarly low. A Joint Advisory Committee to Congress found that less than 1% of total U.S. provider locations use e-care. Approximately 200 e-care networks connect only 3,000 providers across the country; typically, the networks are used on a limited basis.37 A 2008 American Hospital Association survey found that for each of six conditions, only 2-12% of hospitals use Internet-enabled monitoring devices (fixed and mobile), covering 4-8% of relevant patient populations for each condition.38 Only 17% of home-care agencies use remote monitoring solutions in their practices.39
Significant Government Action
The federal government has launched a set of major health IT initiatives to overcome some of the barriers preventing the use of technology, with the goal of transforming America’s health care. The largest step by far is a $19 billion net investment to incent the meaningful use of certified EHR technology.
This action is transformative for two reasons: the investment is substantial, and the funding mechanism is focused on measurable outcomes, not inputs. Physicians can earn up to $44,000 in extra Medicare payments from 2011 to 2015 if they become meaningful users of EHRs; hospitals can collect an initial bonus and an extra payment each time a Medicare patient is discharged.40 There is a similar scheme for Medicaid providers. Rather than provide physicians grants to purchase software, computers and broadband, a set of outcomes such as e-prescribing, data exchange and capturing quality measurements defines “meaningful use.”41 Participants determine the best way to achieve those outcomes. To further adoption, incentives give way to penalties for those that fail to meaningfully use EHRs by 2015.
It is important to recognize the radical change in this approach. The health care delivery system has been dogged for years by criticism that incentives are not aligned to outcomes. The meaningful use mechanism is an attempt, supported by an enormous federal investment and the threat of financial penalties, to develop a new incentive model.
In addition to these incentives, more than $2 billion has been allocated to help the EHR transition succeed. A nationwide network of Regional Extension Centers is being launched to support physician practices as they adopt EHRs; states are being supported to develop policies and technologies that facilitate trusted health information exchange among providers and institutions; and more than a dozen Beacon Communities are being funded to showcase the program’s potential, while providing important outcome data and implementation lessons.
All these actions were authorized by the Health Information Technology for Economic and Clinical Health (HITECH) Act, which was part of the American Recovery and Reinvestment Act of 2009.42 The HITECH Act provisions were designed to improve individuals’ health and the performance of the health care system. They focus on four basic goals: define meaningful use, encourage and support the attainment of meaningful use through incentives and grant programs, bolster public trust in electronic information systems by ensuring their privacy and security and foster continued health IT innovation.43 The HITECH is implemented by two agencies within HHS: ONC and CMS.
Despite government actions, three gaps remain: adoption, information utilization and connectivity. These gaps must be filled to accelerate the benefits of broadband. Many fall outside the FCC’s traditional purview. For those areas—adoption and data utilization—this chapter highlights some of the most pressing issues and offers high-level recommendations for moving the country forward. Hopefully Congress and the federal agencies responsible for these issues can use these ideas as a starting point or to reinforce efforts underway.
10.3 CLOSING THE BROABAND-ENABLED HEALTH IT ADOPTION GAP
Create Appropriate Incentives for Health IT Utilization
A key barrier to greater broadband-enabled health IT adoption is misaligned incentives.44 Those who benefit most from use of these technologies are often not the same as those who shoulder the implementation costs. Providers are expected to pay for equipment and training and adjust to altered workflows. These costs often outweigh the direct benefits they can reasonably expect to gain in terms of reimbursement for services facilitated by health IT.45 As a result, hospitals and physicians cite funding and unclear investment returns as major barriers to electronic health record adoption.46
Instead, it is payors and patients who reap most of the direct benefits of health IT.47 For example, the federal government—as the payor for veterans’ health care—saves money by using a robust e-care program to avoid hospital admissions and expensive home-based care.48 If a private hospital had implemented a similar program, it might have lost money—forgoing revenue earned through admissions and home-based care services.49
The health IT industry has long looked to the country’s largest payor, CMS, to lead the way in correcting this incentive imbalance. If CMS were to pay providers more for using effective health IT solutions, all sides would benefit: providers could practice 21st century medicine without losing money ; patients could receive 21st century care and achieve better health outcomes ; and CMS could save money over time.
Unfortunately, the fee-for-service reimbursement mechanism is not an effective means for realizing health IT’s benefits. Fee-for-service rewards providers for volume, and more reimbursement under such a model exposes CMS to the risk of higher costs absent demonstrated health improvements.50 Coupled with budget neutrality restrictions, it is difficult for CMS to incent broader health IT adoption under this scheme.
HHS’s meaningful use approach addresses the incentive misalignment problem for EHRs by moving to outcomes-based reimbursement. Outcomes-based reimbursement alleviates the incentive problem by tying payments to proven, measurable expenditure reductions and health improvements.51 However, no such systematic solution has been offered for e-care. Currently, CMS only reimburses about $2 million in telehealth services52 from a budget that exceeds $300 billion.53
Recommendation 10.1: Congress and the Secretary of Health and Human Services (HHS) should consider developeing a strategy that documents the proven value of e-care technologies, proposes reimbursement reforms that incent their meaningful use and charts a path for their widespread adoption.
HHS is moving toward outcomes-based reimbursement to stimulate EHR adoption and is well positioned to do the same for e-care. A clearly articulated e-care strategy will accomplish two main purposes:
- Marshal support from Congress, states and the health care community to drive e-care use.
- Provide the health IT industry with a clear understanding of the federal government’s policies toward e-care.
In crafting an e-care strategy, HHS should consider developing new payment platforms to drive adoption of applications proven to be effective. It should also support evaluation of nascent e-care technologies through pilots and demonstration projects. In the course of this effort, HHS should look for opportunities to broaden reimbursement of e-care under the current fee-for-service model. After a reasonable timeframe, Congress should consider convening a panel to review HHS’s recommendations and taking action to ensure these technologies’ wider adoption. The National Broadband Plan recommends including the following steps as part of this initiative:
1. HHS should identify e-care applications whose use could be immediately incented through outcomes-based reimbursement.In its recommendations to Congress, HHS should prioritize e-care applications that it believes are proven to warrant reimbursement incentives. Using the same rigor applied to meaningful use of EHRs, HHS should define these applications’ use cases, data requirements and associated outcomes (expenditure reductions and health improvements). Models such as the VHA’s e-care pilot, for instance, could be codified into concrete use cases and criteria for gauging outcomes. These could then be translated into CMS reimbursement incentives for demonstrating meaningful use of the technologies and achieving specified outcomes.
Future iterations of the meaningful use program could offer one means for implementing these reimbursement changes. Draft 2013 and 2015 meaningful use standards require EHRs to be capable of leveraging certain e-care technologies. However, as currently worded, these requirements will not address modifying reimbursement to incent e-care utilization.54
2. When testing new payment models, HHS should explicitly include e-care applications and evaluate their impact on the models. Where proven and scalable, these alternative payment models would provide an additional solution for incenting e-care. Several alternative payment models have been proposed by the Medicare Payment Advisory Commission and through the health care legislative process. Tests of these models, which are in various stages of implementation, offer an ideal venue for understanding the role e-care can play in outcomes-based reimbursement. Tests include Acute Care Episode Demonstration,55 Medicare Medical Home Demonstration,56 Independence at Home, Patient-Centered Medical Home, Accountable Care Organization pilots and Bundled Payment pilots.57 These pilots and demonstration projects could include an explicit objective to identify e-care use cases and evaluate their effect on health outcomes and expenditure reductions. For instance, in an Independence at Home pilot, remote monitoring could be evaluated as a tool at sample participant sites to understand its impact on quality, data capture and cost savings.
3. For nascent e-care applications, HHS should support further pilots and testing that review their suitability for reimbursement. HHS should champion e-care technology pilots where additional data are needed to evaluate their value. HHS has a number of testing mechanisms that it should use to prove the system-wide potential of e-care. Where possible, major pilots of e-care should be designed to adhere to HHS standards for program design, data capture and other requirements for reimbursement decisions and payment model reform. HHS should collaborate in design stages with parties conducting pilots and provide additional funding when its criteria create extra administrative costs.
There are a number of opportunities for HHS to pursue further pilots:
- HHS should make e-care pilots and demonstration projects a top priority across the agency, including the Health Services Resources Administration, the Substance Abuse and Mental Health Services Administration, IHS,58 NIH and the Agency for Healthcare Research and Quality. HHS-funded projects should be designed with the objectives of understanding use cases, measuring outcomes and determining optimal payment methodologies to produce efficient, high-quality care.
- HHS should collaborate with federally administered providers of care (e.g., VHA, IHS and the Bureau of Prisons) that can act as role models and testbeds for health IT use. For future programs similar to VHA’s e-care program (see Box 10-3), HHS should become involved early on to ensure that programs are designed appropriately to inform reimbursement decisions and payment model reform.
- Large-scale private pilots of e-care such as the Connected Care Telehealth Program in Colorado59 and the Community Partnerships and Mobile Telehealth to Transform Research in Elder Care60 should similarly consult with HHS and share valuable lessons learned. For pilots that meet HHS’s data collection standards, Congress should consider tax breaks or other incentives. For example, Medicare Advantage plan administrators could receive tax credits for testing e-care within their Medicare populations.
The FCC should use data from e-care pilots to update its understanding of health care institutions’ broadband requirements. Pilots showcasing emerging technologies that will be used more widely in the subsequent 10 years will be good opportunities to test the network demands of those technologies. Updated use requirements should be coupled with periodically updated reviews of the country’s state of connectivity (both wired and wireless) to give the public and other government agencies a better understanding of potential health care broadband gaps. (See Section 10.5 for further recommendations on the FCC’s role in monitoring health care broadband.)
4. As outcomes-based payment reform is developed, CMS should seek to proactively reimburse for e-care technologies under current payment models. While outcomes-based reimbursement is the optimal payment model for realizing the potential of e-care, it will be years before payment reform transforms the U.S. health care delivery system. In the meantime, CMS should proactively seek means for reimbursing e-care under the current fee-for-service model. This might include the following:
- Collaborating with physicians, researchers, vendors and government stakeholders to design tests that will prove system-wide expenditure reduction under CMS’s fee-for-service model.
- Widening coverage for currently reimbursed use cases where they have been proven to reduce system-wide expenditures.
- Providing feedback to the community of physicians, researchers and vendors who are trying to enact solutions. Through greater decision-making transparency, CMS could provide critical information that allows that community to target its efforts where they matter most.
- Incenting Medicare Advantage plans to invest rebates (the difference between the established price of care for enrollees and the benchmark for care in that county, of which 75% must be invested as mandatory, health-related supplemental benefits) in the adoption of e-care technologies. Incentives should stipulate tracking health outcomes and expenditure reductions associated with use of these technologies (in compliance with HHS’s tracking guidelines).
- Incenting Home Health Agencies reimbursed through CMS to use e-care technologies where CMS believes the technologies will create better health outcomes and reduced expenditures, while requiring participants to track impact associated with the supported technologies.
Physician associations and vendors have recommended areas where they believe expanded reimbursement of e-care, under the current fee-for-service model, will reduce overall CMS expenditures while expanding access to care.61 As long as the fee-for-service model is the standard, the onus remains on these stakeholders to meet CMS’s criteria to expand reimbursement. Examples such as the Veterans Affairs program are less relevant in this case because they operate under a closed payment system. However, CMS’s review board should ensure it fully analyzes the system-wide benefits of e-care when making reimbursement decisions.
Modernize Regulation to Enable Health IT Adoption
There is a wide range of problems around the legal and regulatory framework that underpins the use of health IT.62 Outdated laws and regulations inhibit adoption, and regulatory uncertainty deters investments in both innovation and utilization.
Recommendation 10.2: Congress, states and the Centers for Medicare & Medicaid Services (CMS) should consider reducing regulatory barriers that inhibit adoption of health IT solutions.
Several rules have not kept up with technology changes and inhibit adoption of e-care and other health IT solutions. They include the following:
- Credentialing and privileging. CMS should revise standards that make credentialing and privileging overly burdensome for e-care; such standards conflict with the goal of expanding access to care. A hospital is not allowed to use the decisions of another hospital as the basis for credentialing and granting privileges; rather, hospitals must conduct their own assessments. For e-care, this means the site where a patient is located (the originating site) may not rely on the site where the physician is located (the distant site) for credentialing and privileging the doctor prescribing care and must instead follow the same process used to credential and privilege any other physician on staff.63 It can be expensive and time-consuming for originating sites to identify and grant privileges to all the physicians treating its patients via e-care, and they often lack the in-house expertise to privilege specialists. It also creates an undue burden on remote physicians to maintain privileges at numerous additional hospitals and limits the pool of experts a hospital may access. The additional complexity and expense from these standards inhibit e-care. CMS should engage the e-care community and other experts to explore national standards or processes that facilitate e-care while protecting patient safety and ensuring accountability for care.
- State licensing requirements. States should revise licensing requirements to enable e-care. State-by-state licensing requirements limit practitioners’ ability to treat patients across state lines. This hinders access to care, especially for residents of states that do not have needed expertise in-state. For example, the national ratio for developmental-behavioral pediatricians is 0.6 per 100,000 children; 27 states fall below that level.64 The increase in autism-spectrum condition diagnoses creates greater demand for this scarce subspecialty. The nation’s governors and state legislatures could collaborate through such groups as the National Governors Association, the National Conference of State Legislatures and the Federation of State Medical Boards to craft an interstate agreement.65 If states fail to develop reasonable e-care licensing policies over the next 18 months, Congress should consider intervening to ensure that Medicare and Medicaid beneficiaries are not denied the benefits of e-care.
- E-prescribing. Congress and states should consider lifting restrictions that limit broader acceptance of electronic prescribing, a technology that could eliminate more than two million adverse drug events and 190,000 hospitalizations, as well as save the U.S. health care system $44 billion per year.66 One set of rules that needs to be addressed relates to the ban on e-prescribing of controlled substances such as certain pain medications and antidepressants. Drug Enforcement Administration rules require doctors to maintain two systems: a paper-and-fax-based system for auditing controlled substances and an electronic system for other drugs. The complexity of dual systems is at best an inconvenience and at worst an impediment to adoption.67 Although a pilot to test e-prescribing of controlled substances is pending, stricter security requirements may prove too burdensome and inhibit adoption. Furthermore, the solution for e-prescribing controlled substances must be compatible with EHRs certified to meet meaningful use criteria. Failure to resolve security protocols and interoperability issues for controlled substances may further delay widespread adoption of e-prescribing.
Recommendation 10.3: The FCC and the Food and Drug Administration (FDA) should clarify regulatory requirements and the approval process for converged communications and health care devices.
The use of communications devices and networks in the provision of health care is increasing. Smartphones have become useful tools for many physicians managing patient care on the go. Medical devices68 increasingly rely on commercial wireless networks to relay information for patient health monitoring and decision support. Some examples of the convergence between communications and medicine include the following:
- Mobile applications that help individuals manage their asthma, obesity or diabetes
- A smartphone application that displays real-time fetal heartbeat and maternal contraction data allowing obstetricians to track a mother’s labor
- An iPhone application that presents images for clinicians making appendicitis diagnoses
- Wearable wireless patch-like sensors that transmit health data over commercial wireless networks to practitioners, caregivers and patients
These and other products cover a broad range of health IT solutions. At one end, general-purpose communications devices such as smartphones, video-conferencing equipment and wireless routers are regulated solely by the FCC when not created or intended for medical purposes. At the other, medical devices, including life-critical wireless devices such as remotely controlled drug-release mechanisms, are regulated by the FDA. However, the growing variety of medical applications that leverage communications networks and devices to transmit information or to provide decision support to both clinicians and consumers presents challenges to the current federal regulatory regime. Potential lack of clarity about the appropriate regulatory approach to these convergent technologies threatens to stifle innovation, slow application approval processes and deter adoption.
The FCC and the FDA should collaborate to address and clarify the appropriate regulatory approach for these evolving technologies. As part of this process, the FCC and the FDA should seek formal public input within the next 120 days and hold a workshop with representatives from industry and other relevant stakeholders to examine real case studies. Through this joint, transparent process the agencies should seek to answer questions such as: “Which components of a health solution present risk that must be regulated?” “How can the process for introducing products to the market be improved?” and “What are the characteristics needed for ‘medical-grade’ wireless?” After public input is received, the agencies should offer joint guidance to address these and other relevant questions.
The FCC and the FDA are committed to working together to facilitate innovation and protect public health in the continued development of safe and effective convergent devices and systems.
10.4 UNLOCKING THE VALUE OF DATA
Data are becoming the world’s most valuable commodity. In multiple sectors—including finance, retail and advertising—free-flowing and interoperable data have increased competition, improved customer understanding, driven innovation and improved decision-making. Fortune 500 companies such as Google and Amazon have based their business models on the importance of unlocking data and using them in ways that produce far-reaching changes.
In personal finance, for example, individuals can share their data from multiple bank accounts, credit cards and brokerage accounts with trusted third parties. These parties provide personalized services that benefit consumers, such as credit card recommendations that tailor reward programs to a customer’s spending patterns.
The advanced use of data in health care offers immense promise in many areas:
- Better treatment evaluations. Therapeutic drugs are not tested across all relevant populations. For example, pharmaceutical companies do not conduct widespread tests of new drugs on children for ethical and practical reasons. But increasingly, physicians are treating them with medications that were designed for adults. This may be the right treatment, but, too often, no one knows. The federal government, recognizing the need for better data in comparing treatment options, has recently allocated $1.1 billion toward comparative effectiveness research.69 Health IT can further this priority. By using applications to collect and analyze the existing data, which today are locked in paper charts, physicians and researchers can evaluate the efficacy and side effects of treatments from disparate groups of patients in order to develop best practices.
- Personalized medicine. Many therapeutic drugs are indiscriminately applied to vast populations without sufficient understanding of which treatments work better or worse on certain people. Genomic research produces huge amounts of data that, when combined with clinical data, could enable development of better targeted drugs. Such drugs could improve outcomes and reduce side effects.
- Enhanced public health. Accurately measuring health status, identifying trends and tracking outbreaks and the spread of infectious disease at a population level are extremely difficult. Health IT enables widespread data capture, which in turn allows better real-time health surveillance and improved response time to update care recommendations, allocate health resources and contain population-wide health threats.
- Empowered consumers. Consumers are too often passive recipients of care, not accessing, understanding or acting upon their own data. Health IT applications that provide easy access and simplify vast amounts of data empower consumers to proactively manage their health. Empowered consumers better grasp their health needs, demand high-quality services and make informed choices about treatment options.
- Improved policy decisions. Innovation in health care delivery systems and payment models is stifled by the lack of suitable interoperable data. The prevailing health care payment model mainly pays for volume of services rendered rather than quality of services provided. However, the right data will help make outcomes-based reimbursement possible by allowing consumers, payors and providers to understand the impact of various prevention and treatment options.
Digital health care in America is at an inflection point. The HITECH Act should vastly improve both the capture of interoperable clinical data and consumer access to such data. Nevertheless, a number of barriers prevent the advanced use of data to make Americans healthier for less money. First, not all types of health data are uniformly captured and interoperable. Second, government regulations continue to limit consumer access to personal health data.
Box 10-4: Data Advance Medicine and Public Health70
The Framingham Heart Study (FHS), which focused on cardiovascular disease (CVD), illustrates how widespread data capture, aggregation, sharing and analysis can transform medicine.
By 1948, when the study was initiated, cardiovascular disease had become an epidemic in the U.S. Death rates for CVD had been on the rise for half a century, but little was known about the causes of heart disease and strokes. The study began with a group of more than 5,200 men and women who provided detailed medical histories and underwent physical exams, lab tests and lifestyle interviews every two years since joining the study. The data were initially painstakingly captured in written form. Today the study spans three generations of participants, totals nearly 15,000 lives and the data are available online.
FHS is cited as the seminal study in understanding heart disease. The data collected made possible fundamental changes in its knowledge base and treatment. For example, FHS led to the identification and quantification of CVD risk factors—high blood pressure, high blood cholesterol, smoking, obesity, diabetes and physical inactivity. CVD risk factors are now an integral part of modern medical curricula and have facilitated the development of novel therapeutics and effective preventive and treatment strategies in clinical practice. FHS has led to the publication of approximately 1,200 research articles in leading journals.71
Broadband will enable the capture of digital health information for all diseases, from patients across the country. Wider availability and analysis of such rich data will allow similar studies for numerous other conditions and populations to be conducted easier and faster. This could broadly transform understanding of disease risk factors and treatment options.
Recommendation 10.4: The Office of the National Coordinator for Health Information Technology (ONC) should establish common standards and protocols for sharing administrative, research and clinical data, and provide incentives for their use.
Digital health data are difficult to collect and aggregate. Such data generally are held in proprietary “siloed” systems that do not communicate with one another and therefore cannot be easily exchanged, aggregated or analyzed. The meaningful use incentives for electronic health records will greatly increase the capture of interoperable clinical health information. However, the inability of researchers to access clinical data in standard format and in a secure manner hinders clinical breakthroughs. Performing research across an amalgamation of all types of health care data will remain a challenge absent uniform data standards.
Coordinated standards and protocols will likely increase innovation and discovery within basic science research, clinical research and public health research, helping alleviate many failings of the health care system. The analysis of combined genomic, clinical and real-time physiological data (often captured wirelessly) could help researchers better understand the interplay of genetics and the environment. This could result in personalized interventions based on associations between people and their surroundings, leading to better outcomes.
Combined administrative and clinical data could be an invaluable tool for shifting to an outcomes-based reimbursement system, as well as providing the ability to build statistical models outlining the economic and clinical effects of novel health policy prior to implementation.
The vision is to enable a continuously learning and adaptive health care system that ubiquitously collects information, aggregates it and allows real-time analysis and action. Extending data interoperability to administrative and research data is possible without creating a centralized database controlled by government or private sector actors. But significant administrative, privacy, technology and financial concerns must be resolved in order to empower decentralized solutions. While developing new versions of meaningful use, ONC is best positioned to convene a group of experts across the public and private sectors to address these difficult issues and develop a path forward. ONC should move to extend data interoperability standards.
Recommendation 10.5: Congress should consider providing consumers access to—and control over—all their digital health care data in machine-readable formats in a timely manner and at a reasonable cost.
There are too many barriers between consumers and their health data, including administrative, diagnostic, lab and medication data. For example, in Alabama it can take up to 60 days to receive medical records and cost $1 per page for the first 25 pages of those records.72 The Health Insurance Portability and Accountability Act (HIPAA) gave individuals the right to access their protected health information, and the recent HITECH Act broadened this right by allowing individuals to obtain a copy of their records digitally within 96 hours of the provider obtaining the information. Both were important steps. However, depending on the nature of the data, there are barriers preventing consumer access. Lab results, for example, may only be released to “authorized persons,” which often excludes the patient, despite their requests. In contrast, consumers can access their prescription medication lists from their treating physicians or individual pharmacies that have patient portals, but not from e-prescribing intermediaries that aggregate much of this data. The latter is not a regulatory problem; rather, it is due to a lack of incentives for payors, pharmacy benefit managers and pharmacies to allow e-prescribing intermediaries to disseminate the information.
But it is consumers’ data. A troubling statistic is that patients are not informed of approximately 7% of abnormal lab results.73 Consumers armed with the right information could do a better job managing their own health, demanding higher quality services from their providers and payors and making more informed choices about care.74 With seamless access to their raw health data, including lab data and prescriptions, consumers could plug the information into specialized applications of their choice and get personalized solutions for an untold number of conditions (See Box 10-5).
Innovation within this space is occurring from the ground up and it is impossible to predict the potential of future applications. What is certain is that in order to maximize innovation and further personalization of health care, consumers must be able to have access to all their health care data and the right to provide it to third- party application developers or service providers of their choice.75 Congress should consider updating HIPAA, with suitable exceptions,76 to include consumers as “authorized persons” of their digital lab data. In a similar vein, barriers relevant to all other forms of health data should be examined and removed.
Box 10-5: AsthmaMD: A Case Study in the Power of Consumer Health Data
A newly released smartphone application offers a glimpse of the potential when consumers enter even a small amount of data.77 AsthmaMD helps patients manage their asthma by inputting a number of parameters, including current medications, and attack timing and severity. Users can opt to share their data anonymously with the service. The data are aggregated and analyzed with the aim of better understanding the disease, as well as providing specific personalized solutions for the consumer. For example, the application can help users better understand the effectiveness of different medications for asthma management and offer insights into specific triggers for that individual’s attacks (e.g., pollen, dust, exercise). The application also can track the consumer’s precise location and the timing of their asthma activity, which can be correlated with local pollutant count, adverse weather changes and different types of pollutants. In addition, it can alert users with higher risks of an attack in real time if it detects users with a similar asthma history reporting asthma issues. Ultimately it could send live Twitter streams showing geographic areas with asthma flare-ups in real time.
10.5 CLOSING THE HEALTH IT BROADBAND CONNECTIVITY GAP
Characterizing and Sizing the Gap
Research is scarce on health care providers’ broadband connectivity needs and the ability of the country’s infrastructure to meet those needs. This plan is one of the first attempts to quantify both. A number of challenges that prevented earlier study are relevant to this analysis. Pricing data, for instance, are proprietary and fluctuate widely according to a number of variables, making it difficult to quantify an aggregate price curve. Databases of practice locations bear inconsistent category classifications and often overlap (e.g., a small hospital may also be called a rural health clinic; a small health clinic may also be called a medium-sized physician office). Despite these shortcomings, this analysis is necessary to inform health care policy changes related to broadband, including the effort underway to reform the FCC’s Rural Health Care Program.
Health Care Providers’ Broadband Needs
Health care providers’ broadband needs are largely driven by the rapidly increasing amount of digital health-related data that is collected and exchanged. A single video consultation session can require a symmetric 2 Mbps connection with a good quality of service.78 There is a wide range of requirements to support EHRs and medical imaging. Exhibit 10-B shows the variation in file sizes for common health care file types. Over the next decade, physicians will need to exchange increasingly large files as new technologies such as 3D imaging become more prevalent.
Exhibit 10-B: Health Data File Sizes79
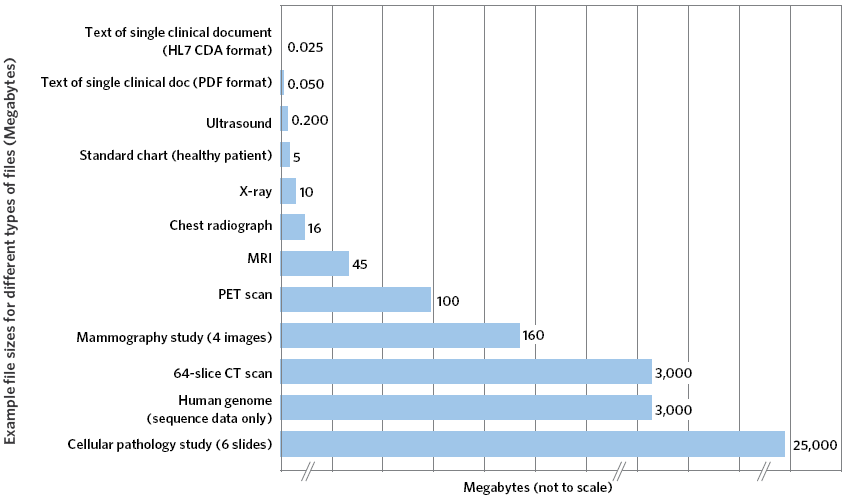
Exhibit 10-C: Required Broadband Connectivity and Quality Metrics (Actual)80
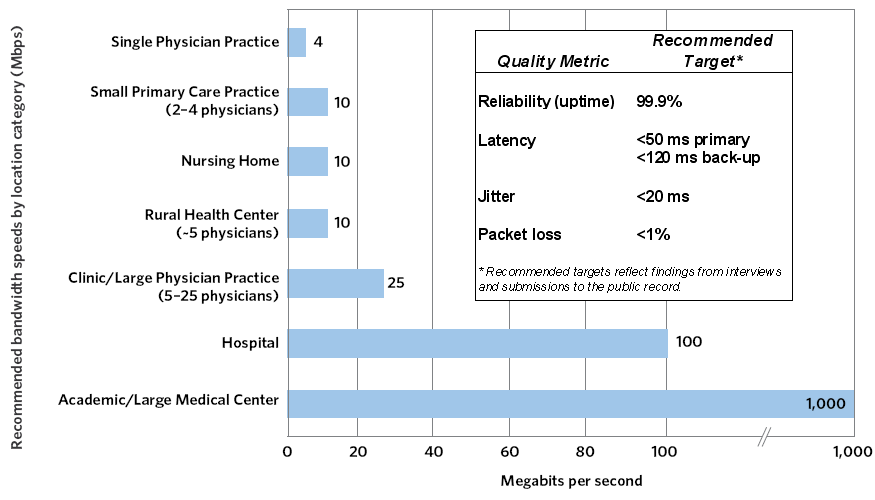
The connectivity needs of different health delivery settings will vary depending on their type (e.g., tertiary care center versus primary care physician practice) and their size. In addition, applications that integrate real-time image manipulation and live video will stimulate demand for more and better broadband,81 because these applications have specific requirements for network speeds, delay and jitter. Exhibit 10-C shows an estimate of the required minimum connectivity and quality metrics to support deployment of health IT applications today and in the near future at different types of health delivery settings. Although some delivery settings currently function at lower connectivity and quality, those levels are straining under increasing demand and are unable to support needs likely to emerge in the near future.82
Most businesses in the United States, physician offices included, have two choices of broadband service categories: mass-market “small business” solutions83 or Dedicated Internet Access (DIA),84 such as T-1 or Gigabit Ethernet service. DIA solutions include broader and stricter Service Level Agreements (SLAs) by network operators. DIA services are substantially more expensive than mass-market packages. For example, in Los Angeles, 10 Mbps Ethernet service with an SLA averages $1,044/month,85 while Time Warner Cable’s similar mass-market package, Business Class Professional, which offers 10 Mbps download speeds and 2 Mbps upload speeds, is approximately $400/month.86
Connectivity Gap: Small Providers (Four or Fewer Physicians)
In general, smaller providers can achieve satisfactory health IT adoption with mass-market “small business” packages of at least 4 Mbps for single physician practices and 10 Mbps for two-to-four physician practices, even though these solutions may not provide business-grade quality-of-service guarantees.87 Since most small physician offices do not provide acute care services, they do not require the same degree of instant and guaranteed responsiveness that large practices and hospitals require.
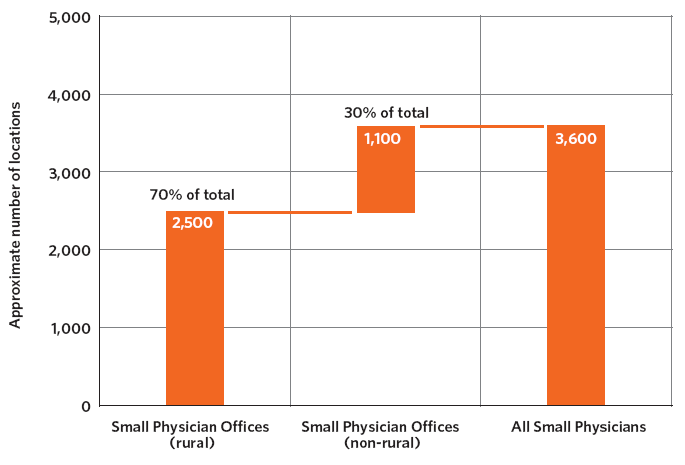
Based on the requirements listed above, an estimated 3,600 out of approximately 307,000 small providers face a broadband connectivity gap. The gap is particularly wide among providers in rural areas (See Exhibit 10-D). In locations defined as rural by the FCC, approximately 7% of small physician offices are estimated to face a connectivity gap. In contrast, across all locations, only approximately 1% of physician offices face a connectivity gap.88
Exhibit 10-D: Estimate of Small Physician Locations Without Mass-Market Broadband Availability89
Connectivity Gap: Medium & Large Providers (Five or More Physicians)
Larger physician offices, clinics and hospitals face connectivity barriers of a different nature. Because of their size and service offerings, these providers often cannot rely on mass-market broadband and must usually purchase DIA solutions. DIA pricing is determined on a case-by-case basis depending on factors such as capacity, type and length of the connection; type of service provider; and type of facility used. It often varies significantly by geography. Exhibit 10-E illustrates how widely DIA prices fluctuate in urban areas.
Exhibit 10-E: Wide Fluctuations in Dedicated Internet Access Prices (Monthly Service Cost in Dollars)91
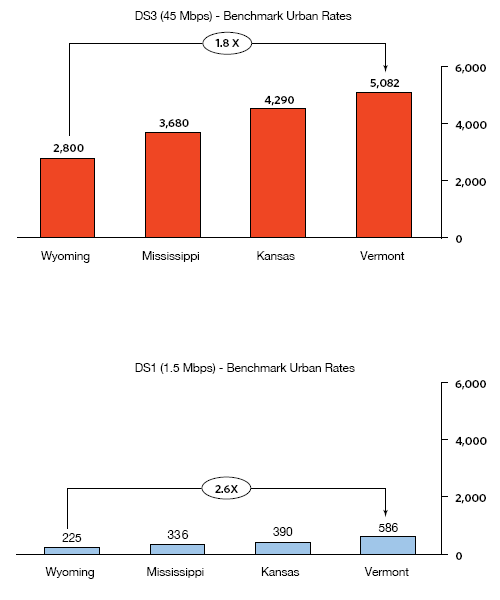
For two large physician offices seeking to capitalize on meaningful use incentives, a disparity of more than $27,000 per year90 in broadband costs puts one at a disadvantage to the other, negates a significant portion of the incentives and may prove an insurmountable obstacle to EHR adoption.
Rural and Tribal areas are likely to face even greater price inequities. There are more than 2,000 rural providers participating in the FCC’s Telecommunications Fund, and their broadband prices average three times the price of urban benchmarks.92
Connectivity Gap: Federally Funded Providers
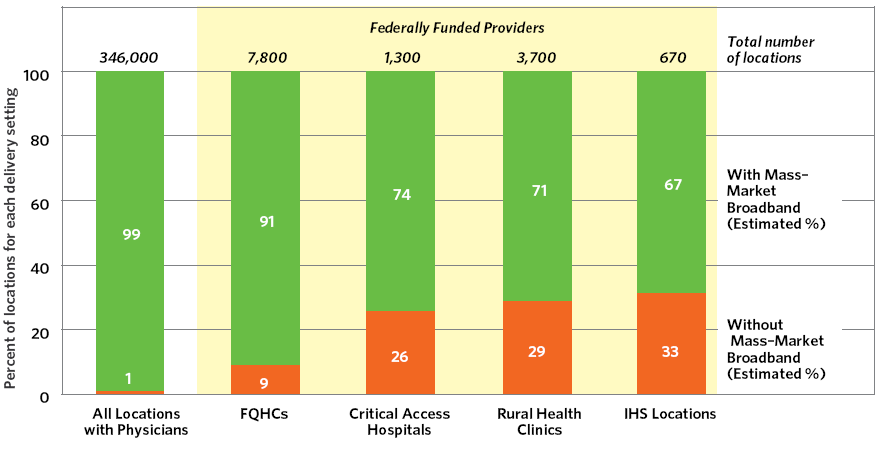
Several federally funded providers93 have insufficient connectivity. For example, 92% of IHS sites purchase a DIA connection of 1.5 Mbps or less.94 These bandwidth constraints prevent IHS providers from achieving full adoption of video consultation, remote image diagnostic and EHR technology. Similarly, federal subsidy recipients such as Federally Qualified Health Centers,95 Rural Health Clinics 96 and Critical Access Hospitals97 face challenges in securing broadband solutions relative to the rest of the country. Exhibit 10-F shows the FCC’s estimate of these providers’ mass-market broadband gaps. It is important to note that these gaps in mass-market broadband do not preclude locations from purchasing DIA solutions. Nearly every IHS location purchases DIA broadband. However, the fact that such high percentages of federally funded providers are located outside the mass-market footprint means that they face significantly higher prices.
Federally funded providers have a direct impact on the government’s costs and serve health care populations for whom the government assumes responsibility; the federal government should improve their connectivity and make them models of harnessing health IT to ensure better health (see Recommendation 10.10).
Exhibit 10-F: Health Care Locations Without Mass-Market Broadband Availability98
Connectivity Gap: Next Phase of Analysis
Understanding the state of broadband connectivity for health care providers is a new but important area of analysis. There is more to be done, especially as the need for better data continues to grow. As nascent health IT applications become more prevalent and the importance of wireless connectivity grows, an up-to-date understanding of broadband use cases and connectivity levels will be invaluable. Immediate efforts should be made to quantify the price disparity problem on a more granular level. Similarly, the levels—and costs—of broadband that providers purchase warrant further analysis.
The FCC should play an ongoing role in serving this knowledge base via the Health Care Broadband Status Report proposed in Recommendation 10.11. This information is important not only to policymakers and regulators, but to the health IT industry and the health care provider community. These groups are also invested in understanding the role broadband plays in health care delivery and should participate in shaping this body of research.
Reform the Rural Health Care Program
The recommendations throughout this plan will have a tremendous impact on health care institutions, particularly the consumers and small providers that will likely be using mass-market solutions. However, because of health care’s role in the lives of consumers and its importance to the national economy, it is critical to retain a dedicated set of programs within USF to help spur broadband adoption by health care providers. The FCC’s Rural Health Care Program as currently structured, however, is not meeting the country’s needs.
In 1997, the FCC implemented the directives of the Telecommunications Act of 1996 by creating a Rural Health Care Program, funded through the USF.99 The program provides three types of subsidies to public and non-profit health care providers. First, the program subsidizes the rates paid by rural health care providers for telecommunications services to eliminate the rural/urban price difference within each state (the Telecommunications Fund).100 Second, to support advanced telecommunications and information services the program provides a 25% flat discount on monthly Internet access for rural health care providers and a 50% discount for health care providers in states that are entirely rural (via the Internet Access Fund).101 Lastly, the FCC adopted a three-year program that provides support for up to 85% of the costs associated with deploying broadband health care networks in a state or region (via the Pilot Program).102 The Pilot Program funds one-time capital costs for network deployment, as well as recurring capital and operational costs over five years.
Exhibit 10-G: 2009 Rural Health Care Program Spending
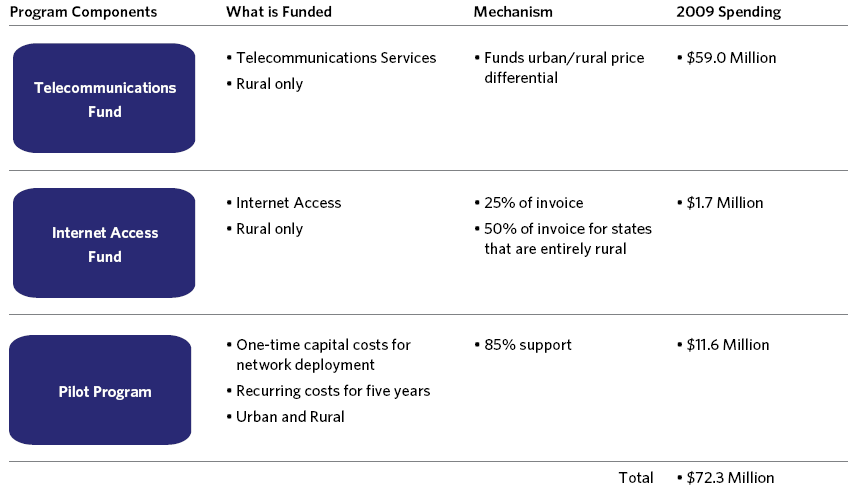
Problems with the Current Program
As previous sections demonstrate, many health care providers have difficulty accessing broadband services because they are located in areas that lack sufficient infrastructure or areas where broadband service is significantly more expensive. Less than 25% of the approximately 11,000 eligible institutions are participating in the program,103 and many are not acquiring connections capable of meeting their needs.104 In 2009, 82% of Telecommunications Fund spending supported connections of 4 Mbps or less,105 which is a minimum for single physician practices that are using a robust suite of broadband-enabled health IT. That speed is increasingly insufficient for the clinics and hospitals that are the major participants in the program.
Thousands of eligible rural health care providers currently do not take advantage of this program. Some claim that this is because the subsidy is too low and the application process is too complex to justify participation.106 Large gaps in broadband access and price disparities for broadband services suggest that change is needed in the support program. Statutory restrictions that limit support to public and non-profit entities and program rules that limit support to rural entities should be re-examined. Many deserving health care providers, such as urban health clinics and for-profit physician offices that function as the safety net for the country’s care delivery system, should become eligible for funding under the program.107 In rural areas alone, for-profit eligibility restrictions exclude more than 70% of the 38,000 health care providers; many face the same disadvantages in securing broadband as the eligible providers.108
The Pilot Program represents an important first step in extending broadband infrastructure to unserved and underserved areas, and ensuring that health care providers in rural areas and Tribal lands are connected with sophisticated medical centers in urban areas. Over 35% of projects have received funding commitments to date. Much of this progress has come in the last 12 months. Extensive outreach from the FCC and efforts of program participants have resulted in funding commitment letters for 22 projects, for a total of $44.5 million.109 To ensure that each program participant has ample time to finalize its project, the FCC has extended the deadline for funding commitment submissions. It should continue to assist participants to ensure networks are built as quickly and effectively as possible.
Despite the FCC’s efforts to date, many health care providers remain under-connected. The FCC’s programs are in need of improved performance measures to assess their impact on broadband services and, more importantly, patient care. The FCC should take a fresh look and evaluate how it can improve the Rural Health Care Program to ensure that funds are used efficiently and appropriately to address the adoption and deployment challenges outlined above. In doing so, lessons learned from the Rural Health Care Pilot Program should be incorporated into this examination.
Recommendation 10.6: The FCC should replace the existing Internet Access Fund with a Health Care Broadband Access Fund.
The Health Care Broadband Access Fund should support bundles of services, including bundled telecommunications, broadband and broadband Internet access services for eligible health care providers. This program would replace the existing underutilized Internet Access Fund. Health care providers eligible to participate in the new program should include both rural and urban health care providers, based on need. The FCC should develop new discount levels based on criteria that address such factors as:
- Price discrepancies for similar broadband services between health care providers
- Ability to pay for broadband services (i.e., affordability)
- Lack of broadband access, or affordable broadband, in the highest HPSAs of the country
- Public or safety net institution status110
To allow health care providers to afford higher bandwidth broadband services, the subsidy support amount under the Health Care Broadband Access Fund should be greater than the current 25% subsidy support under the Internet Access Fund. In addition, support should better match the costs of services for disadvantaged health care providers. To better encourage participation, the FCC should also simplify the application process and provide clarity on the level of support that providers can reasonably expect, while protecting against potential waste, fraud and abuse.
After approximately three years of data collection for the new Health Care Broadband Access Fund, the FCC should examine, based on the success of that program, whether the Telecommunications Fund program needs to be adjusted.
Recommendation 10.7: The FCC should establish a Health Care Broadband Infrastructure Fund to subsidize network deployment to health care delivery locations where existing networks are insufficient.
Many health care providers are located in areas that lack adequate physical broadband infrastructure. Specifically, as demonstrated by the overwhelming interest in the Pilot Program, the FCC was able to identify and begin addressing the lack of access to appropriate broadband infrastructure throughout the nation. The FCC should permanently continue this effort by creating a Health Care Broadband Infrastructure Fund, incorporating lessons learned from administering the Pilot Program. In particular, the Pilot Program has enabled the FCC to obtain valuable data on how to better target support to deploy health care networks where the need is most acute. The following recommendations are based on preliminary lessons from the Pilot Program.
The FCC should establish demonstrated-need criteria to ensure that deployment funding is focused in those areas of the country where the existing broadband infrastructure is insufficient. For example, demonstrated-need criteria could include any combination of the following:
- Demonstration that the health care provider is located in an area where sufficient broadband is unavailable or unaffordable. The forthcoming BDIA broadband map should be a factor in determining availability.
- A financial analysis that demonstrates that network deployment will be significantly less expensive over a specified time period (e.g., 15–20 years) than purchasing services from an existing network carrier.
- Certification that the health care provider has posted for services under the Telecommunications Funds and/or the Internet Access Fund (or the new Health Care Broadband Access Fund) for an extended period of time (for example, six-to-twelve months) and has not received any viable proposals from qualified network vendors for such services.
The FCC should also:
- Require that program participants pay no less than a minimum percentage of all eligible project costs, such as the 15% match requirement used in the Pilot Program. The match contribution requirement aligns incentives and helps ensure that the health care provider values the broadband services being developed and makes financially prudent decisions regarding the project.
- Facilitate efficient use of USF-funded infrastructure. For the Pilot Program, the FCC has required that any excess capacity (broadband capacity in excess of the amount required for the eligible health care providers) must be paid for by the health care provider or a third party, at fair share.111 Fair share has been defined as a proportionate share of all costs, including trenching and rights-of-way. In instances where excess capacity will be used by other USF eligible institutions, the FCC should allow the excess capacity to be paid for by those institutions at incremental cost rather than fair share. The FCC should also explore ways to encourage joint applications between eligible health care providers and other USF-qualifying institutions, such as schools and libraries.
- Simplify the community buildout fair share rules so non-USF eligible institutions can accurately and efficiently estimate their proper share of network deployment costs and join the infrastructure projects. It is in a community’s best interest when public, non-profit and private institutions share infrastructure costs and bring broadband to more of the community. The FCC should define, early in the process, permissible ways in which excess capacity can be deployed and allocated to non-USF-eligible institutions.
- Maintain existing criteria utilized in the Pilot Program, including requirements that projects are sustainable, create statewide or regional networks and leverage existing network technology. Moreover, the FCC should continue to allow (but not require) the connection of networks to proprietary nationwide backbones that link government research institutions and academic, public and private health care providers that house significant medical expertise.
- Simplify program application and administration. For example, the FCC should allow some limited funding of project administration costs for network design and project planning.
The FCC should set a target for how much yearly support should go to infrastructure versus ongoing support. Based on the benefits these programs can deliver to American health care, the FCC should plan to spend up to the current annual cap and then consider additional funding if the need exists and funds can be made available.
Recommendation 10.8: The FCC should authorize participation in the Health Care Broadband Funds by long-term care facilities, off-site administrative offices, data centers and other similar locations. Congress should consider providing support for for-profit institutions that serve particularly vulnerable populations.
The term “health care provider” has been interpreted narrowly, excluding, for example, nursing homes, hospices, other long-term care facilities, off-site administrative offices and health information data centers.112 The FCC should re-examine that decision in light of trends in the health care landscape and expand the definition to include, where consistent with the statute, those institutions that have become integral in the delivery of care in the United States. The expanded definition of eligible health care providers should explicitly include off-site administrative offices of eligible health care providers, long-term care facilities, data centers used for health care purposes and owned (directly or indirectly) by eligible health care providers, dialysis centers and skilled nursing facilities.
The FCC should periodically look to the ONC (e.g., every two years) to determine whether the definition of institutions eligible for funding as an eligible health care provider should be changed while the health IT landscape evolves.
In addition, Congress should consider expanding the definition of health care providers eligible for USF funding to include certain for-profit entities.113 Under the Communications Act, eligibility for funding under the Rural Health Care Program is limited to public or non-profit entities.114 Not supporting private and for-profit health care providers has a significant impact on some important components of the health delivery system that serve needy populations. In rural areas, for example, private physician clinics can be the most critical—and sometimes the only—health care delivery location in the community. The power of digitized patient records is most valuable when all providers, including private physicians, are connected.
Including for-profit locations will require appropriate limitations to ensure that money from USF is targeted to health care providers that serve particularly vulnerable populations. For instance, funding for health IT in the Recovery Act is available to private physicians that either bill Medicare or have patient volumes consisting of at least 30% Medicaid beneficiaries (20% for pediatricians).115 This methodology could provide Congress a template to consider for expanding USF eligibility.
Recommendation 10.9: To protect against waste, fraud and abuse in the Rural Health Care Program, the FCC should require participating institutions to meet outcomes-based performance measures to qualify for USF subsidies, such as HHS’s meaningful use criteria.
The FCC should align its health care program with other federal government criteria intended to measure the efficient use of health IT, such as the meaningful use criteria being developed by HHS.116 This will help ensure the FCC’s programs encourage physicians and hospitals to not only deploy networks or purchase broadband services, but to use them in a way that improves the country’s health delivery system. For example, participants in the FCC programs should be required to achieve meaningful use certification for EHRs, after a certain period of support (e.g., three years).
The FCC should work with HHS (and other relevant agencies) and seek comment from the public to determine which outcome metrics (e.g., coordination with Regional Extension Centers, remote monitoring of chronic patients) should be utilized to assess its programs’ impact on broadband usage and the delivery of medicine at participating locations. For metrics that are deemed particularly difficult to attain, the FCC should consider offering additional support to those health care providers that are most successful in utilizing broadband services to improve the lives of their patients.
By following the path Congress laid out in the HITECH Act and re-focusing federal investments away from process and toward outcomes (specifically meaningful use of health IT), the FCC can contribute to an important transformation of federal spending. Most importantly, it can ensure that the program funds not just wires, but health. Also, it can allow the FCC to give program participants more authority over project administration as long as they are achieving well-defined objectives. The FCC should evaluate and improve upon its oversight (e.g., competitive bidding, audits and investigations) to ensure that funds are being used to further the statutory purposes of universal service and doing the most to impact broadband usage and the delivery of medicine, while minimizing waste, fraud and abuse.
Recommendation 10.10: Congress should consider providing an incremental sum (up to $29 million a year) for the Indian Health Service for the purpose of upgrading its broadband service to meet connectivity requirements.
The Indian Health Service offers a unique opportunity for Congress to consider taking action. There is a clear need for broadband—many IHS sites are extremely remote and Tribal lands generally have low broadband penetration rates (see Exhibit 10-F). Since IHS is an integrated system that directly impacts the federal government’s bottom line,117 taxpayers stand to realize the savings and efficiency improvements promised by best-practice health IT utilization across IHS. IHS can serve as a testbed for forward-looking health IT use, much as VHA does with its CCHT program.118
Congress should consider providing additional public funding for IHS locations that currently have insufficient levels of broadband connectivity. IHS estimates that the annual expenditure to upgrade its broadband service is $29 million.119 New funding should be contingent on a competitive process that ensures efficient use of funds and clear goals tied to the meaningful use of health IT, as outlined in the proposed reforms for the Health Care Broadband Access Fund. Where new infrastructure needs to be deployed, it should be deployed in a way that maximizes value for the surrounding communities, providing low-cost, high-speed infrastructure where it did not previously exist.
After one year of administering the IHS funding, Congress should consider doing the same for other federally funded providers with a connectivity gap. Where Congress does not act directly, these networks of providers should remain a high priority for the FCC’s reformed Health Care Broadband Access and Infrastructure programs.
Recommendation 10.11: The FCC should periodically publish a Health Care Broadband Status Report.
Health IT is in its infancy. The private sector innovations and public programs described in this chapter are merely an overview of the explosion in activity. While the National Broadband Plan lays the path forward, it will be critical for the FCC to play a more prominent and sustained role in evaluating broadband infrastructure and in supporting the nation’s health transformation. The health care connectivity analysis should serve as a starting point for measuring the health care connectivity problem and assessing the effectiveness of potential solutions.
The FCC should publish a Health Care Broadband Status Report every two years. It should discuss the state of health care broadband connectivity, review health IT industry trends, describe government programs and make reform recommendations. For the FCC’s programs, these analyses should be coupled with a dedicated effort to assess their impact on broadband usage and health care delivery at participating locations. The Rural Health Care Program has improved access to quality medical services, but the FCC lacks comprehensive information to determine how funding actually changes behavior. In conjunction with HHS, which has experience evaluating the effectiveness of clinical programs, the FCC should look for better ways to test the impact of the Health Care Broadband Access and Health Care Broadband Infrastructure funds. For instance, the FCC could conduct the following tests:
- Determine how unsupported health care providers differ from supported providers in the utilization of e-care
- Assess the impact of changing the level of broadband subsidies to a targeted community and determine if there is an increased use of broadband and health IT as a result of such subsidies
- Explore whether including funding for training would lead to better broadband utilization and improved care
- Evaluate the impact the program is having on vulnerable populations, such as the elderly, racial and ethnic minorities or low-income rural and urban communities, to understand whether targeted efforts would be more effective
Through these mechanisms, the FCC should develop a culture of testing and learning. Working in conjunction with participants, policymakers and industry leaders, the FCC should seek to continuously evaluate the impact of its programs and change direction when they do not meet expectations. To ensure sufficient support for these tests, the FCC should allocate a portion of the existing funding cap (e.g., $5 million) for innovative ideas or programs that can evaluate existing efforts or improve upon them in the future. These actions could also help reduce waste, fraud and abuse, because program effectiveness could be continuously monitored, with rules and administration adjusted as necessary.
As technologies rapidly evolve, so too do expectations for health IT adoption in America. Supporting health IT requires further analysis of complex issues and the development of solutions to address them. The work ahead will be most successful if it combines the efforts of government, industry and the health care community.
1 Ctr. for Medicare & Medicaid Serv., National Health Expenditure Projections 2008–2018, http://www.cms.hhs.gov/NationalHealthExpendData/downloads/proj2008.pdf (last visited Jan. 21, 2010).
2 Office of the Surgeon General, Overweight and Obesity: At a Glance, http://www.surgeongeneral.gov/topics/obesity/calltoaction/fact_glance.htm (last visited Jan. 21, 2010). Obesity is a particular challenge for African Americans, as approximately four out of five African American women are overweight or obese. See Department of Health and Human Services, Office of Minority Health, http://minorityhealth.hhs.gov/templates/content.aspx?ID=6456 (last visited Feb. 28, 2010). In addition, African American adults are twice as likely as non-Hispanic white adults to have been diagnosed with diabetes by a physician, and in 2005, African American men were 30% more likely to die from heart disease, as compared to non-Hispanic white men. See Department of Health and Human Services, Office of Minority Health, http://minorityhealth.hhs.gov/templates/browse.aspx?lvl=2&lvlID=51 (last visited Feb. 28, 2010).
3 Susan Dentzer, Reform Chronic Illness Care? Yes, We Can, 28 Health Aff. 12, 12 (Jan./Feb. 2009), available at http://content.healthaffairs.org/cgi/reprint/28/1/12.
4 Shin-Yi Wu & Anthony Green, RAND Corp., Projection of Chronic Illness Prevalence and Cost Inflation (2000).
5 Am. Heart Ass’n, Heart Failure, http://www.americanheart.org/chf (last visited Jan. 21, 2010)
6 Inst. of Medicine, Preventing Medical Errors 5 (Philip Aspden et al. eds., 2007), available at http://books.nap.edu/openbook.php?record_id=11623&page=5.
7 Robert A. Weinstein, Nosocomial Infection Update, 4 Emerging Infectious Disease 416 (July–Sept. 1998), available at ftp://ftp.cdc.gov/pub/EID/vol4no3/adobe/weinstein.pdf.
8 See Health Res. & Serv. Admin., U.S. Dep’t of Health & Human Serv., The Physician Workforce: Projections and Research into Current Issues Affecting Supply and Demand (2008), ftp://ftp.hrsa.gov/bhpr/workforce/physicianworkforce.pdf (HRSA, Physician Workforce); Michael J. Dill & Edwa rd S. Salsberg, Ass’n of Am. Med. Coll., The Complexities of Physician Supply and Demand: Projections Through 2025, at 6 (2008) (estimating a shortage of 124,000 physicians by 2025), https://services.aamc.org/publications/index.cfm?fuseaction=Product.displayForm&prd_id=244 (download report from this page).
9 HRSA, Physician Workforce at iv.
10 Institute of Medicine, Unequal Treatment: Confronting Racial And Ethnic Disparities In Health Care 29 (Brian Smedley et al. eds., 2003.)
11 Id.
12 Medicare and Medicaid Programs; Electronic Health Record Incentive Program; Proposed Rule, 75 Fed. Reg. 1851 (Jan. 13, 2010).
13 This is not a definitive taxonomy. Electronic health record definition used by Health Information and Management Systems Society (HIMSS). See HIMSS, Electronic Health Record, http://www.himss.org/ASP/topics_ehr.asp (last visited Feb. 27, 2010).
14 Todd Park & Peter Basch, Ctr. for Am. Progress, A Historic Opportunity: Wedding Health Information Technology to Care Delivery Innovation and Provider Payment Reform 6 (2009), available at http://www.americanprogress.org/issues/2009/05/pdf/health_it.pdf (Park & Basch, Wedding Health Information Technology).
15 See Catherine DesRoches et al., Electronic Health Records in Ambulatory Care—A National Survey of Physicians, 359 New Eng. J. Med. 50 (2008), available at http://content.nejm.org/cgi/reprint/359/1/50.pdf.
16 James Bigelow et al., RAND Corp., Analysis of Healthcare Interventions That Change Patient Trajectories, at xxiv (2005). http://www.rand.org/pubs/monographs/2005/RAND_MG408.pdf.
17 Richard Hillestad et al., Can Electronic Medical Record Systems Transform Healthcare? Potential Health Benefits, Savings, and Costs, 24 Health Aff. 1103, 1103 (Sept./Oct. 2005), available at http://content.healthaffairs.org/cgi/reprint/24/5/1103.
18 Hillestad et al., Can Electronic Medical Record Systems Transform Healthcare? at 1114.
19 American Academy of Pediatrics Comments in re NBP PN #17 (Comment Sought on the Health Care Delivery Elements of National Broadband Plan—NBP Public Notice #17, GN Docket Nos. 09-47, 09-51, 09-137, Public Notice, 24 FCC Red 137 28 (WCB 2009) (NBP PN #17)), filed Dec. 4, 2009, at 1; Rural Wisconsin Health Cooperative Information Technology Network (RWHC ITN) Comments in re NBP PN #17, filed Dec. 4, 2009, at 3.
20 Sixty-five million people reside in Primary Care Health Professional Shortage Areas (HPSAs). HHS designates HPSAs as having a shortage of primary medical care, dental, or mental health providers. They may be urban or rural areas, population groups, or medical or other public facilities. See HRSA, Shortage Designation: HPSAs, MUAs & MUPs, http://bhpr.hrsa.gov/shortage/ (last visited Jan. 29, 2010).
21 Lee Schwamm et al., Recommendations for the Implementation of Telemedicine within Stroke Systems of Care: A Policy Statement from the American Heart Association, 40 Stroke 2635 (2009), available at http://stroke.ahajournals.org/cgi/reprint/40/7/2635. The United States has approximately 4.0 neurologists per 100,000 persons, who ideally need to be caring for over 780,000 acute strokes per year, and many parts of the country lack access to acute stroke services entirely. Id. at 2638. Tissue plasminogen activator (tPA) is a clot-busting drug that must be administered within 3 hours of ischemic stroke onset to be effective. Id. at 2641.
22 Richard Knox, Drug Can Stop Strokes, But Most Patients Don't Get It,NPR, Dec. 14, 2009, http://www.npr.org/templates/story/story.php?storyId=121032269&sc=emaf.
23 Store-and-forward technologies represent the collection and storage of clinical data or images that are forwarded for interpretation at a time distant from an in-person clinical encounter. Ctr. for Info. Tech. Leadership, Health Care Information and Management Systems Society (HIMSS), The Value of Provider-to-Provider Telehealth Technologies (2007) (CITL, The Value of Provider-to-Provider Telehealth Technologies), available at http://www.citl.org/_pdf/CITL_Telehealth_Report.pdf.
24 CITL, The Value of Provider-to-Provider Telehealth Technologies. CITL modeled pre- and post-telehealth costs based on national baseline number of transports, transport cost, and number of avoided transports. Annual savings were calculated by subtracting post-telehealth costs from pre-telehealth costs for each provider-to-provider setting. These savings sum to $1.2 billion.
25 Juan M. Aranda, Jr. et al., Current Trends in Heart Failure Readmission Rates: Analysis of Medicare Data, 32 Clinical Cardiology 47, 47 (2009), available at http://www3.interscience.wiley.com/cgi-bin/fulltext/121637973/PDFSTART.
26 Robert Litan, Better Health Care Together Coalition, Vital Signs Via Broadband: Remote Health Monitoring Transmits Savings, Enhances Lives (2008), available at http://www.betterhealthcaretogether.org/Library/Documents/VITAL%20SIGNS%20via%20BROADBAND%20FINAL%20with%20FOREWORD%20and%20TITLE%20pp%2010%2022.pdf
27 Adam Darkins et al., Care Coordination/Home Telehealth: The Systematic Implementation of Health Informatics, Home Telehealth, and Disease Management to Support the Care of Veteran Patients with Chronic Conditions, 10 Telemed. & e-Health 1118, 1118 (2008), available at http://www.liebertonline.com/doi/pdf/10.1089/tmj.2008.0021?cookieSet=1.
28 Qualcomm Inc. Comments in re NBP PN #17, filed Dec. 4, 2009, at 20.
29 Body sensor networks are very short-range networks consisting of multiple body-worn sensors and/or nodes and a nearby hub station. The sensors and/or nodes take readings of key patient-specific information, such as temperature, pulse, blood glucose level, the heart’s electrical activity, blood pressure, and respiratory function. Antenna components embedded in the sensors and/or nodes make it possible to wirelessly transmit data to body-worn or closely-located hub devices. Hub devices may process the data locally and/or transmit it wirelessly for centralized processing, display, and storage.
30 West Wireless Health Institute Comments in re NBP PN #17, filed Dec. 4, 2009, at 2.
31 West Wireless Health Institute Comments in re NBP PN #17, filed Dec. 4, 2009, at 5.
32 Wireless cardiovascular solutions are designed to enable early detection, prevention, and treatment of cardiovascular conditions. These solutions consist of wearable sensors, global wireless capabilities, and comprehensive web-based infrastructures. See, e.g., Corventis Home Page, http://www.corventis.com/US/ (last visited Jan. 30, 2009).
33 Medtronic, REAL-Time Continuous Glucose Monitoring, http://www.minimed.com/products/insulinpumps/components/cgm.html (last visited Feb. 1, 2010).
34 Amendment of Parts 2 and 95 of the Commission’s Rules to Establish the Medical Micropower Network Service in the 413–457 MHz Band, RM-11404, Petition for Rulemaking (filed Sept. 5, 2007).
35 Letter from Cheryl A. Tritt, Counsel to the Alfred Mann Foundation, Morrison & Foerster LLP, to Marlene H. Dortch, Secretary, FCC, ET Docket No. 09-36 (Feb. 2, 2010) (Alfred Mann Feb. 2, 2010 Ex Parte) at 12.
36 Cathy Schoen & Robin Osborn, The Commonwealth Fund, The Commonwealth Fund 2009 International Health Policy Survey of Primary Care Physicians in Eleven Countries 10 (2009), http://www.commonwealthfund.org/~/media/Files/Publications/In%20the%20Literature/2009/Nov/PDF_Schoen_2009_Commonwealth_Fund_11country_intl_survey_chartpack_white_bkgd_PF.pdf. Count of 14 functions includes: (1) electronic medical record; (2, 3) electronic prescribing and ordering of tests; (4–6) electronic access to test results, Rx alerts, and clinical notes; (7–10) computerized system for tracking lab tests, guidelines, alerts to provide patients with test results, and preventive/follow-up care reminders; and (11–14) computerized list of patients by diagnosis, by medications, and due for tests or preventive care.
37 Joint Advisory Committee on Communications Capabilities of Emergency Medical and Public Health Care Facilities, Report to Congress (2008), available at http://energycommerce.house.gov/Press_110/JAC.Report_FINAL%20Jan.3.2008.pdf.
38 Hospitals & Health Networks, Figure 10: Home Telemonitoring, http://www.hhnmag.com/hhnmag_app/jsp/articledisplay.jsp?dcrpath=HHNMAG/Article/data/07JUL2008/0807HHN_MW_MainArticle_Fig10&domain=HHNMAG (last visited Jan. 30, 2010).
39 Phillips, National Study on the Future of Technology and Telehealth in Home Care 105 (2008).
40 David Blumenthal, Launching HITECH, New Eng. J. Med., Dec. 30, 2009, at 3, (Blumenthal, Launching HITECH) available at http://content.nejm.org/cgi/reprint/NEJMp0912825v1.pdf.
41 HIT Policy Committee, Meaningful Use Objectives and Measures: 2011-2013-2015 (early version) (2009), http://healthit.hhs.gov/portal/server.pt/gateway/PTARGS_0_10741_887553_0_0_18/Proposed_Revisions_to_Meaningful_Use_ post_7_16_2009_FINAL_PT1_508.pdf.
42 American Recovery and Reinvestment Act of 2009, Pub. L. No. 111-5, § 13101, 123 Stat. 115, 231 (2009) (Recovery Act).
43 Blumenthal, Launching HITECH, at 3.
44Park & Basch, Wedding Health Information Technology at 2, 5–7, 14; Medicare Payment Advisory Comm’n (MedPAC), Report to the Congress: Promoting Greater Efficiency in Medicare 17 (2007), available at http://www.medpac.gov/documents/jun07_EntireReport.pdf; Great Call, Inc. Comments in re NBP PN #17, filed Dec. 4, 2009, at 7; Palmetto State Providers Network Comments in re PN #17, filed Nov. 24, 2009, at 12 (filed by W. Roger Poston, II)
45 Cal. Telemed. and eHealth Ctr., Optimizing Telehealth in California: An Agenda for Today and Tomorrow 4–7 (2009) (CTEC, Optimizing Telehealth in California), available at http://www.cteconline.org/_pdf/Findings-Report.pdf.
46 Ashish K. Jha et al., Use of Electronic Health Records in U.S. Hospitals, 360 New Eng. J. Med. 1628 (2009), available at http://content.nejm.org/cgi/reprint/360/16/1628.pdf.
47 CTEC, Optimizing Telehealth in California at 4.
48 See Box 10.3, supra.
49 Park & Basch, Wedding Health Information Technology at 2, 5–7, 14.
50 MedPAC, Report to the Congress: Medicare in Rural America 36 (2001), available at http://www.medpac.gov/documents/Jun01%20Entire%20report.pdf.
51 Park & Basch, Wedding Health Information Technology at 2, 5–7, 14.
52 CMS uses the term telehealth, which is similar to the term e-care. See Box 10.1 for further explanation.
53 Payment Policies Under the Physician Fee Schedule and Other Revisions to Part B for CY 2010, 74 Fed. Reg. 33519, 33663 (July 13, 2009) (codified at 42 C.F.R. pts. 410, 411, 414, etc.), available at http://edocket.access.gpo.gov/2009/E9-15835.htm; Office of the Nat’l Coordinator for Health Info. Tech., HHS, Justification of Estimates for Appropriations Committees: Fiscal Year 2011 (2010), available at http://healthit.hhs.gov/portal/server.pt/gateway/PTARGS_0_11673_910512_0_0_18/ONC_FY2011_CJ.pdf.
54 For instance, the Health IT Policy Council cites “Incorporate data from home monitoring device” as one of the objectives for defining Meaningful Use in 2013. HIT Policy Committee, Meaningful Use Objectives and Measures: 2011-2013-2015 (final version) 6 (2009), available at http://healthit.hhs.gov/portal/server.pt/gateway/PTARGS_0_10741_888532_0_0_18/FINAL%20MU%20RECOMMENDATIONS%20TABLE.pdf.
55 CMS, CMS Announces Demonstration to Encourage Greater Collaboration and Improve Quality Using Bundled Hospital Payments (press release), May 16, 2008, available at http://www.cms.hhs.gov/apps/media/press/release.asp?Counter=3109&intNumPerPage=10&checkDate=&checkKey=&srchType=1&numDays=3500&srchOpt=0&srchData=&keywordType=All&chkNewsType=1%2C+2%2C+3%2C+4%2C+5&intPage=&showAll=&pYear=&year=&desc=&cboOrder=date.
56 CMS, Medical Home Demonstration Fact Sheet (2009), http://www.cms.hhs.gov/demoprojectsevalrpts/downloads/medhome_factsheet.pdf.
57 See Patient Protection and Affordable Care Act, H.R. 3590, 111th Cong. §§ 2703, 3022–24 (2009), available at http://frwebgate.access.gpo.gov/cgi-bin/getdoc.cgi?dbname=111_cong_bills&docid=f:h3590eas.txt.pdf; Affordable Health Care for America Act, H.R. 3962, §§ 1152, 1301–02, 1312 (2009), available at http://docs.house.gov/rules/health/111_ahcaa.pdf.
58 IHS is an agency within the Department of Health and Human Services responsible for providing federal health services to 1.9 million American Indians and Alaska Natives in predominantly rural and remote areas. Indian Health Service, IHS Fact Sheets Year 2009 Profile, http://info.ihs.gov/Profile09.asp (last visited Dec. 29, 2009).
59 The Connected Care Telehealth Program is a pilot of video consultation services—sponsored by UnitedHealth Group, Cisco, Centura Health, the Colorado Rural Health Center and the Colorado Community Health Network—that will make available 4,800 remote specialist visits per year in Colorado. UnitedHealthcare, UnitedHealthcare to Launch Connected Care Telehealth Program in Rural Colorado (press release) (Apr. 17, 2009), http://www.connectedcareamerica.com/news-and-resources.php (link available to the article from this page).
60 The Community Partnerships and Mobile Telehealth to Transform Research in Elder Care is a National Institute of Health Challenge Grant awarded to the University of Virginia to test connecting seniors to health IT applications.
61 American Telemedicine Association Comments in re NBP PN #17, filed Dec. 3, 2009, at 14.
62 Letter from Alice Borrelli, Director, Global Healthcare and Workforce Policy, Intel Corporation, to Marlene H. Dortch, Secretary, FCC, GN Docket Nos. 09-57, 09-51, 09-137 (Dec. 16, 2009) (Intel Dec. 16, 2009 Ex Parte) at 32.
63 The Joint Commission (TJC), which accredits roughly 82% of the nation’s hospitals, is permitted by CMS to implement a proxy process for credentialing between TJC-accredited hospitals. This leaves the new privileging requirement for TJC-accredited hospitals, and both the credentialing and privileging requirements for non-TJC accredited hospitals. Telehealth Leadership Initiative, Question and Answer: Credentialing and Privileging of Telehealth Providers, http://www.telehealthleadership.org/Credentialing%20Privileging%20Q&A%20.DOC (last visited Jan. 30, 2010).
64 Nat’l Ass’n of Children’s Hospitals & Related Inst., National Shortages of Pediatric Subspecialists Impede Children’s Access to Care (press release), Jan. 13, 2010, available at http://www.childrenshospitals.net/AM/Template.cfm?Section=Home3&CONTENTID=49773&TEMPLATE=/CM/ContentDisplay.cfm.
65 American Telemedicine Association Comments in re NBP PN #17, filed Dec. 3, 2009, at 16.
66 Ctr. for Info. Tech. Leadership, The Value of Computerized Provider Order Entry in Ambulatory Settings: Executive Preview 6–7 (2009), http://www.citl.org/research/ACPOE_Executive_Preview.pdf.
67 John Moore, Doctors and the DEA, Gov’t Health IT, Oct. 1, 2008, http://www.govhealthit.com/newsitem.aspx?tid=77&nid=69394.
68 See FDA, Medical Devices, Is the Product a Medical Device?, http://www.fda.gov/MedicalDevices/DeviceRegulationandGuidance/Overview/ClassifyYourDevice/ucm051512.htm (last visited Jan. 30, 2010) (providing the FDA definition of a medical device).
69 HHS, Comparative Effectiveness Research Funding, http://www.hhs.gov/recovery/programs/cer/index.html (last visited Feb. 20, 2010)
70 See Framingham Heart Study, About the Framingham Heart Study, http://www.framinghamheartstudy.org/about/index.html (last visited Feb. 19, 2010) (providing an overview of the Framingham Heart Study).
71 Am. Heart Ass’n, Framingham Heart Study, http://www.americanheart.org/presenter.jhtml?identifier=4666 (last visited Feb. 20, 2010).
72 Joy Pritts & Nina L. Kudszus, Health Pol’y. Ins., Your Medical Record Rights in Alabama (A Guide to Consumer Rights Under HIPAA), available at http://medicalrecordrights.georgetown.edu/stateguides/al/al.pdf.
73 Lawrence P. Casalino et al., Frequency of Failure to Inform Patients of Clinically Significant Outpatient Test Results, 169 Arch Intern Med. 1123, 1123 (2009), available at http://archinte.ama-assn.org/cgi/reprint/169/12/1123.
74 See Sharon B. Arnold, Acad. Health & Robert Wood Johnson Found., Improving Quality Health Care: The Role of Consumer Engagement (2007).
75 See supra Chapter 4.
76 There are sensible exemptions, which can be found at 45 C.F.R. § 164.524(a)(3). See citation for more circumstances whereby a covered entity can deny access but individuals also have a right to request a review of the denial.
77 See Michael Arrington, AsthmaMD Helps Asthma Sufferers, Gathers Aggregate Research Data, TechCrunch, Jan. 10, 2010, http://www.techcrunch.com/2010/01/10/asthmamd-helps-asthma-sufferers-gathers-aggregate-research-data/.
78 Letter from Chuck Parker, Executive Director, Continua Health Alliance, to Marlene H. Dortch, Secretary, FCC, GN Docket Nos. 09-57, 09-51 (Nov. 16, 2009) (Continua Nov. 16, 2009 Ex Parte) Attach. at 13. Bandwidth thresholds are actual (i.e., not advertised) speeds.
79 GE Healthcare Comments in re NBP PN #17, filed Dec. 4, 2009, at 8; Euclid Seeram, Digital Image Compression, Radiologic Tech., July–Aug. 2005, http://www.entrepreneur.com/tradejournals/article/134676840.html; Human Genome Project Information, Frequently Asked Questions, http://www.ornl.gov/sci/techresources/Human_Genome/faq/faqs1.shtml (last visited Jan. 31, 2010); Ichiro Mori et al., Issues for Application of Virtual Microscopy to Cytoscreening, Perspectives Based on Questionnaire to Japanese Cytotechnologists, Diagnostic Pathology, July 15, 2008, http://www.diagnosticpathology.org/content/pdf/1746-1596-3-S1-S15.pdf. See, e.g., DICOM sample image sets, http://pubimage.hcuge.ch:8080/ (last visited Jan. 31, 2010).
80 Mbps recommendations reflect compilation of the record. Numbers are guidelines, not precise measures. See, e.g., Letter from Alrc Borelli Director Global Healthcare and Workforce Policy Intel, to Marlene H. Dortch, Secretary, FCC, GN Docket Nos. 09–47, 09–51, 09–137, WC Docket No 07–10 (Dec. 16, 2009). See also, e.g., Fiberutilities Group, A Practical Review of Broadband Requirements For Healthcare Clinical Applications 6–7 (2009), available at http://www.fiberutilities.com/documents/FG_Press_Release_FCC_Briefing_Healthcare_Application_Requirements_for_Broadband_110609.pdf.
81 GE Healthcare Comments in re NBP PN #17, filed Dec. 4, 2009, at 2.
82 Ascension Health Comments in re NBP PN #17, filed Dec. 4, 2009, at 5; RWHC ITN Comments in re NBP PN #17, filed Dec. 4, 2009, at 3.
83 AT&T and Verizon both call these offerings “Small Business” offerings. Comcast calls it their “Business Internet Service.” TimeWarner Cable calls it their “Business Class Wideband Internet” service.
84 DIA is used as an umbrella term for all components of monthly broadband service for DSL lines. This includes both circuit and access services.
85 Telegeography, Enterprise Network Pricing Service(Q3 2009). (Regarding methodology, “the Enterprise Network Pricing Service presents and analyzes responses to hypothetical bid scenarios for MPLS IP VPN WAN services. Carriers complete surveys on a bi-annual basis supplying prices for each component of a ten-city wide area network, breaking out core network, equipment and management fees from local access.”). Price cited here is an average of the 5 lowest bids for Los Angeles.
86 TimeWarner Business Class Professional 10 x 2, listed at $399.95 / month on TimeWarner Los Angeles website. Taxes and other surcharges not factored in. See Time Warner Cable Business Class, https://www.twcbc.com/LA/buyflow/buyflow.ashx (last visited Feb. 27, 2010) (requires providing additional information to access).
87 Statement reflects compilation of the record and is a guideline, not a comprehesive requirement. Record in response to NBP PN #17 and ex parte filings (see e.g., Letter from Winfred Y. Wu, Director, Public Health Informatics, New York City Department of Health and Mental Hygiene, to Marlene H. Dortch, Secretary, FCC, GN Docket Nos. 09-47, 09-51, 09-137 (Mar. 1, 2010).
88 Access to mass-market broadband is used here to mean passed by terrestrial broadband access facilities such as those used to deliver DSL or cable modem service. This analysis does not predict how many of the 307,000 small providers purchase the appropriate level of broadband; only the mass-market broadband available to them. The analysis is a predictive estimate combining the FCC’s statistical network model and provider databases, as shown below. Gap is calculated based on connectivity requirement threshold of 4 Mbps for Single Physician Practices and 10 Mbps for all other practices. AMA small provider locations (four physicians or less) were assigned to an appropriate census block, based on their street address, and then reconciled with the model showing connectivity availability for that census block. About 24,000 (or 7%) of the health care locations in the AMA database had addresses that were impossible to convert accurately to census blocks; results for these locations were modeled to complete the analysis. A small percentage of the records (less than 1.5%) were geographically located outside of the Master Broadband Availability data (e.g., Puerto Rico), and therefore were dropped from consideration in the connectivity analysis. The analysis does not take into account other network quality requirements. Some of these locations may have alternative networks or commercial services, where residential broadband is unavailable.
- Omnibus Broadband Initiative (OBI) The Broadband Gap (forthcoming) (OBI, The Broadband Availability Gap).
- Database of all locations in the United States with practicing physicians: Am. Med. Ass’n, AMA Physician Masterfile Database (2009) on file with the FCC, “The Physician Masterfile includes current and historical data for more than 940,000 residents and physicians and approximately 77,000 students in the United States.” Includes all active practicing physicians in the US (655,630) and the addresses where they practice. Sorting by address sorts 655,630 physicians into 351,172 locations, with a size metric for each one based on how many physician entries are associated with each location entry. Removed 5,077 locations in Puerto Rico and other locations that were not included in the Statistical Model, leaving 346,095 locations for our analysis. Detailed information on this database is available from the AMA. AMA Physician Masterfile, http://www.ama-assn.org/ama/pub/about-ama/physician-data-resources/physician-masterfile.shtml (last visited Feb. 27, 2010).
- FCC’s Rural definition, 47 CFR § 54.5: “For purposes of the rural health care universal service support mechanism, a ‘rural area’ is an area that is entirely outside of a Core Based Statistical Area; is within a Core Based Statistical Area that does not have any Urban Area with a population of 25,000 or greater; or is in a Core Based Statistical Area that contains an Urban Area with a population of 25,000 or greater, but is within a specific census tract that itself does not contain any part of a Place or Urban Area with a population of greater than 25,000. ‘Core Based Statistical Area’ and ‘Urban Area’ are as defined by the Census Bureau and ‘Place’ is as identified by the Census Bureau.”
89 See supra note 88.
90 Difference between DS3 purchased in Wyoming versus Vermont for one year of service, according to rates listed in Exhibit 10-e, infra, is $27,384.
91 Wyoming, Mississippi, New York, and Vermont prices: USAC, Urban Rate Search Tool, http://www.usac.org/rhc/tools/rhcdb/UrbanRates/search.asp (last visited Feb. 8, 2010) (use 2009 data). Chicago and Houston prices.
92 Letter from William England, Vice President, Rural Health Care Division, Universal Service Administrative Company, to Marlene H. Dortch, Secretary, FCC, GN Docket Nos. 09-47, 09-51, 09-137 (Feb. 23, 2010) (USAC Feb. 23, 2010 Ex Parte) at 1. If locations in Alaska are excluded, the participants’ broadband price still averages 3x the price of their urban benchmarks.
93 Federally funded providers include provider networks that are directly administered by the federal government (e.g., Veterans Health Administration, NASA, Bureau of Prisons, Indian Health Service), as well as recipients of federal subsidies.
94 See Letter from Theresa Cullen, RADM, U.S. Public Health Service, Chief Information Officer and Director, Indian Health Service, to Marlene H. Dortch, Secretary, FCC, GN Docket Nos. 09-47, 09-51, 09-137 (Feb. 23, 2010) (IHS Feb. 23, 2010 Ex Parte), Attach.
95 “FQHCs are ‘safety net’ providers such as community health centers, public housing centers, and programs serving migrants and the homeless. The main purpose of the FQHC Program is to enhance the provision of primary care services in underserved urban and rural communities.” CMS, Federally Qualified Health Center Fact Sheet 1 (2009), http://www.cms.hhs.gov/MLNProducts/downloads/fqhcfactsheet.pdf. FQHCs qualify for cost-based CMS reimbursement and other benefits.
96 “The Rural Health Clinic Program was established in 1977 to address an inadequate supply of physicians who serve Medicare and Medicaid beneficiaries in rural areas.” CMS, Rural Health Clinic Fact Sheet 1 (2007), http://www.cms.hhs.gov/MLNProducts/Downloads/rhcfactsheet.pdf. Clinics must meet criteria established by HHS, including being located in rural area and in a Health Provider Shortage Area or a Medically Underserved Area. RHC institutions qualify for cost-based CMS reimbursement and other benefits.
97 Critical Access Hospitals are hospitals qualified to receive cost-based reimbursement from Medicare and are important components of states’ rural health networks. See generally CMS, Critical Access Hospitals Fact Sheet (2009) (discussing what qualifies as a Critical Access Hospital), available at http://www.cms.hhs.gov/MLNProducts/downloads/CritAccessHospfctsht.pdf.
98 Access to mass-market broadband is used here to mean passed by terrestrial broadband access facilities such as those used to deliver DSL or cable modem service; business-class service, including business-grade service level agreements, is likely available currently but at much higher prices (potentially including large one time special-construction costs). This analysis does not predict how many of the providers purchase the appropriate level of broadband; only if mass-market broadband is available to them. The analysis is a predictive estimate combining the FCC’s statistical network model and provider databases as shown below. Gap is calculated based on connectivity requirement threshold of 4 Mbps for Single Physician Practices (from either DSL/FTTN or Cable) and 10 Mbps for all other practices (from cable service only). Health care locations were assigned to an appropriate census block, based on their street address, and then reconciled with the model showing connectivity availability for that census block. For each database, a percentage of the health care locations had addresses that were impossible to convert accurately to census blocks; results for these locations were modeled to complete the analysis. For the AMA, this accounted for ~24,000 (or 7%) of total entries. For IHS, this accounted for ~350 (or 52%) of entries. Additionally, the FQHC database contained duplicate location records, which were excluded from the connectivity analysis. A small percentage of the records (less than 1.5%) were geographically located outside of the Master Broadband Availability data (e.g., Puerto Rico), and therefore were dropped from consideration in the connectivity analysis.The analysis does not take into account other network quality requirements. Some of these locations may have alternative networks or commercial services, where residential broadband is unavailable.
• OBI, The Broadband Availability Gap. The OBI deployment team created a nationwide model for broadband availability from wired and wireless technologies. Database of all locations in the United States with practicing physicians: AMA, AMA Physician Masterfile Database (2009) on file with the FCC, “The Physician Masterfile includes current and historical data for more than 940,000 residents and physicians and approximately 77,000 students in the United States.” Includes all active practicing physicians in the US and the addresses where they practice. Sorting by address sorts 655,630 physicians into 346,095 locations, with a size metric for each one based on how many physician entries are associated with each location entry. Removed 5,077 locations in Puerto Rico and other locations that were not included in the Statistical Model, leaving 346,095 locations for our analysis. Detailed information on this database is available from the AMA. AMA Physician Masterfile, http://www.ama-assn.org/ama/pub/about-ama/physician-dataresources/physician-masterfile.shtml (last visited Feb. 27, 2010).
• Federally Qualified Health Center Database: HRSA Electronic Handbooks, Bureau of Primary Health Care Management Information System, Scope Repository retrieved via the HRSA Geospatial Data Warehouse’s Health Care Service Delivery Sites report at http://datawarehouse.hrsa.gov/HGDWReports/RT_App.aspx?rpt=HS, retrieved on Oct. 24, 2009.
• Rural Health Clinic Database: CMS, Name and Address Listing For Rural Health Clinic Database (accessed Oct. 6, 2009). Updated versions are available at http://www.cms.hhs.gov/MLNProducts/downloads/rhclistbyprovidername.pdf.
• Critical Access Hospitals Database: HHS, Health Resources and Services Administration, HRSA Geospatial Data Warehouse—Report Tool, http://datawarehouse.hrsa.gov/HGDWReports/RT_App.aspx?rpt=P2 (providing data snapshot from Sept. 30, 2009).
• IHS Database: IHS Feb. 23, 2010 Ex Parte, Attach.
99 See 47 U.S.C. §§ 254(h)(1)(A), 254(h)(2)(A); 47 C.F.R. Part 54, Sbpt. G—Universal Service Support for Health Care Providers.
100 47 C.F.R. §§ 54.605–613.
101 47 C.F.R. § 54.621.
102 See Rural Health Care Support Mechanism, WC Docket No. 02-60, Order, 21 FCC Rcd 11111 (2006) (2006 Pilot Program Order); Rural Heath Care Support Mechanism, WC Docket No. 02-60, Order, 22 FCC Rcd 20360 (2007) (2007 RHC PP Selection Order).
103 There were 2,570 locations that participated in the FCC’s Rural Health Care Program, excluding the Pilot Program, in 2009. Eligibility was determined by matching the locations of non-public and public institutions with the FCC’s geographic definition of rural. See 47 C.F.R. § 54.5. Estimate of 10,660 unique locations include 1,851 nonprofit hospitals, 2,612 Federally Qualified Health Centers (FQHCs), 3,349 Rural Health Clinics (as defined by HHS), 358 Indian Health Service (by HHS rules, all IHS sites are also FQHCs), 607 Veterans Health Affairs, 106 Federal Prisons (BOP), and 3,219 public health departments. At the time of publication, we did not have addresses for individual BOP and VHA sites, so we assumed a rural/urban split in the same proportions to IHS and hospitals, respectively. Public Health Departments were estimated as one location per county that was deemed totally rural by the FCC. All other locations were geo-coded by census block to determine eligibility. These categories may be inconsistent with FCC terminology, since it has traditionally used its own definition of “hospital” and “rural health clinic.” Also, 10,660 is likely an underestimate of eligible institutions because it does not count community mental health centers, postsecondary medical education, or state prisons.
104 See RWHC ITN Comments in re NBP PN #17, filed Dec. 4, 2009, at 7; USF Consultants Comments in re NBP PN #17, filed Dec. 7, 2009, at 5.
105 USAC Feb. 23, 2010 Ex Parte at 1.
106 See PSPN Comments in re NBP PN#17, filed Dec. 4, 2009, at 13; HNG Comments in re NBP PN#17, filed Dec. 4, 2009, at 5–6; MDH Comments in re NBP PN #17, filed Dec. 4, 2009, at 4; RWHC ITN Comments in re NBP PN #17, filed Dec. 4, 2009, at 7–8.
107 See IHS Comments in re NBP PN #17, filed Dec. 4, 2009, at 13; PSPN Comments in re NBP PN #17, filed Dec. 4, 2009, at 15; PMHA et al. Comments in re NBP PN #17, filed Dec. 4, 2009, at 6; State of New York Comments in re NBP PN #17, filed Dec. 4, 2009, at 12.
108 Total rural health care providers determined by geo-coding of the American Medical Association’s physician master-file (38,403), which includes every location where a licensed physician practices. Am. Med. Ass’n, AMA Physician Masterfile Database (2009). The 10,660 locations that are eligible under the FCC’s Rural Health Program (see endnote 103, supra) only represent 28% of the total locations.
109 FCC, Rural Telemedicine Program Funds 16 More Broadband Telehealth Networks (press release), Feb. 18, 2010, available at http://hraunfoss.fcc.gov/edocs_public/attachmatch/DOC-296348A1.pdf.
110 Safety net institutions are defined by the Health Resource and Services Administration (HRSA). HRSA, HRSA and the Safety-Net, http://answers.hrsa.gov/cgi-bin/hrsa.cfg/php/enduser/std_adp.php?p_faqid=1702&p_created=1243947992&p_topview=1 (last visited Jan. 31, 2010).
111 See 2007 RHC PP Selection Order, 22 FCC Rcd at 20381–82, para. 47.
112 The Rural Health Care Program uses the statutory definition of “health care provider” established in section 254(h)(7)(b) of the 1996 Act, which defines health care providers as: (i) post-secondary educational institutions offering health care instruction, teaching hospitals, and medical schools; (ii) community health centers or health centers providing health care to migrants; (iii) local health departments or agencies; (iv) community mental health centers; (v) not-for-profit hospitals; (vi) rural health clinics; and (vii) consortia of health care providers consisting of one or more entities described in clauses (i) through (vi).
113 See for example, 47 U.S.C. § 254(h)(4), which allows E-rate support to private schools that have an annual endowment of less than $50,000,000.
114 See 47 U.S.C. §§ 254(h)(1)(A), 254(h)(2)(A) (limiting support to public and non-profit health care providers).
115 See also HHS stipulation that any physician (including private practice physicians) can qualify for meaningful use incentives, provided such physicians accepts Medicare or derives more than 20% of their billing from Medicaid patients.
116 The Recovery Act provides Medicare and Medicaid incentive payments to eligible providers, such as physicians and hospitals, in order to increase the adoption of electronic health records (EHRs). To receive the incentive payments, providers must demonstrate “meaningful use” of a certified EHR. Building upon the work done by the HIT Policy Committee, the Centers for Medicare & Medicaid Services (CMS), along with the Office of the National Coordinator for Health Information Technology (ONC), are developing a proposed rule that provides greater detail on the incentive program and proposes a definition of meaningful use. See HHS, Important First Step to Expand the Use of Information Technology to Improve the Health and Care of Every American (press release), June 16, 2009, http://www.hhs.gov/news/press/2009pres/06/20090616a.html.
117 As opposed to, for instance, a private hospital network, where the hospital shareholders directly realize financial gains from using such technologies. In such an example, the government only indirectly realizes the gains, where they result in reductions to overall CMS reimbursements.
118 See Blue Box 10.3, “How Health IT Saves Veterans Affairs Billions Each Year,” supra.
119 IHS Feb. 23, 2010 Ex Parte, Attach. Indian Health Service calculated the annual cost to upgrade its broadband networks to the minimum requirements in Exhibit 10.3, supra. Estimates were made using median prices paid across its 600+ location system. Competitive bidding and selective network deployment similar to the FCC’s universal service programs will likely reduce prices. Also, as Recovery Act funding through BIP and BTOP is spent on Tribal lands, the prices for service may decline.



