2012 Design by Biomedical Undergraduate Teams (DEBUT) Challenge Winners
NIBIB congratulates the winners of the 2012 DEBUT Challenge!
Category: Diagnostic Devices/Methods, winning $10,000
Q-Path: A Flow-Through High-Throughput Quantitative Histology Platform,
University of California Los Angeles Armin Arshi, David Kuo, Robert Lee, Elizabeth
Ng, and Andrew Tan
The fourth most common and ninth most deadly form of cancer in men is bladder cancer,
transitional cell carcinoma (TCC). The Q-Path team developed a high-throughput,
flow-through microfluidic platform combined with automated image analysis software,
which allows for systematic screening of patients’ urine samples in order to noninvasively
diagnose TCC. The system provides the pathologist with a quantitative analysis of
the sample and an index to differentiate between healthy, low-grade malignancy,
and high-grade malignancy. The device has the potential to be applied to a broader
range of bodily fluid samples, including blood and pleural fluids; hence it could
play a key role in the early diagnosis of various types of cancers.
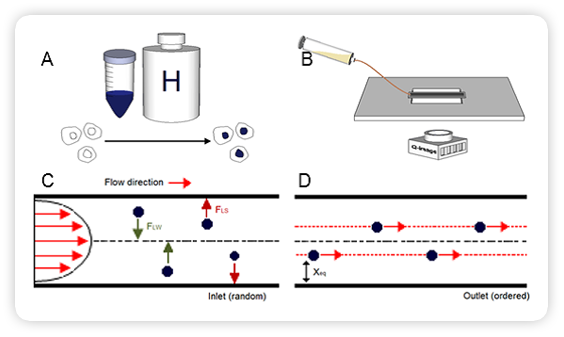
Q-Path high-throughput platform design and implementation (A) Concentrated
cell suspensions were stained to selectively label nuclei and (B)
fed into an inertially focusing microfluidic chip and imaged using high-speed color
microscopy. (C) Inside the channel, cells are subject to a size-dependent
shear gradient lift force (FLS) due to laminar fluid flow and an opposing
wall effect lift force (FLW) due to the channel wall. Cells adopt equilibrium
positions (Xeq) according to size at outlet where they are rapidly imaged.
Category: Therapeutic Devices/Methods, winning $10,000
Quick-Stitch – Surgical Suturing Device to Improve Fascia Closure,
Johns Hopkins University Anvesh Annadanam, Luis Herrera, Haley Huang, Leslie Myint,
Daniel Peng, Andyg Tu, Stephen Van Kooten, Sohail Zahid
Quick-Stitch is an inexpensive, disposable suturing tool for gastrointestinal surgery
that improves safety, efficiency, and consistency in stitching fascia (a collagenous
layer underneath the skin that wraps around the internal organs to keep them from
pressing against the skin layer). The device aims to improve surgeon performance
and patient outcomes by regulating stitch placement and tension, thus helping to
avoid the problems of hernias and ischemia that can result from improper stitching
after gastrointestinal surgery.
Category: Technology to Aid Underserved Populations and Individuals with Disabilities,
winning $10,000
Low-Cost Spirometer, Washington University in St. Louis
Andrew Brimer, Abigail Cohen, Olga Neyman, Charles Yong-Chao Wu, Braden Eliason
There is a lack of devices to measure lung function for the diagnosis and monitoring
of respiratory diseases in the developing world. Traditional spirometers cost in
the range of $1,000-$2,000. The Low-Cost Spirometer team developed a fluidic oscillating
spirometer costing under $10 without compromising accuracy or precision with respiratory
diseases like Chronic Obstructive Pulmonary Disease (COPD) on the rise, the durable,
low-cost spirometer could improve healthcare in the developing, as well as the developed
world.

Low-Cost Spirometer
Honorable Mentions
Category of Diagnostic Devices/Methods
Immunofluidics - Rapid Tissue Typing Diagnostic Chip,
University of California Irvine: Philip Chao, Jay LePere, Daniel Lorey, Brandon
Wong, Irfanali Kermalli
D1GIT: Automated, Temperature-calibrated Measurement of Capillary Refill
Time, University of Pennsylvania: Craig McDonald, Anat Bordoley,
Rikki Irwin, Viraj Kalyani, Dorsey Standish
Category of Therapeutic Devices/Methods
InjectAlign, University of Pennsylvania: Mahesh Murali,
Gabriel Seidner, Michelle Bubear
Shoulder Dislocation Simulator, Northwestern University:
Jin Tao, Sabeen Admani, Faraz Admani
Category of Technology to Aid Underserved Populations and Individuals with Disabilities
Babalung: A Neonatal Apnea Monitor for the Developing World,
Rice University: Jordan Schermerhorn, Rachel Alexander, Rachel Gilbert, Bridget
Ugoh, Andrea Ulrich
Design Of An Eye Tracking System Enabling Communication For TBI And SCI
Patients, University of Denver: Peter Neilson, Jeff Evans, Jordan
Rath, John De Witt
Full project descriptions and videos (if provided) can be viewed at DEBUT.Challenge.gov
NIH DEBUT Press Release
Back to Top
Last Updated On 08/21/2012