Question 2: Does methadone maintenance treatment reduce illicit opioid use?
Answer: Yes. Patients’ illicit opioid use declines, often dramatically, during methadone maintenance treatment. However, adequate methadone dosage and basic psychosocial services are essential for treatment effectiveness.
Research Highlights
Condelli and Dunteman (1993) examined a sample of 526 patients admitted to 17 methadone maintenance treatment programs that participated in the Treatment Outcome Perspective Study (TOPS). This analysis compared the length of methadone maintenance treatment with heroin use. The average short-term treatment duration was 31 days; long-term, 233 days; and continuous, 725 days. The rate of heroin use was 100 percent before treatment, 39 percent after short-term treatment, 40 percent after long-term treatment, and 17 percent after treatment. This study suggests that longer exposure to methadone maintenance treatment decreases the likelihood of heroin use.
A study of 933 heroin addicts participating in methadone maintenance treatment programs compared behavior during periods on and off methadone maintenance. The study demonstrated that during periods on methadone maintenance, illicit narcotic use decreased significantly and reduction in illicit narcotic use was the most prominent effect among nine indicators of treatment success (Powers and Anglin, 1993).
In the Drug Abuse Reporting Program (DARP) study, 44 percent of the 895 patients who entered methadone maintenance treatment reported no daily use of illicit narcotics in the first posttreatment year. This represented a 56-percent decrease from 100-percent daily use in the 2 months before admission (Simpson and Sells, 1982).
Patient Status Before and After Methadone Maintenance Treatment–A study by McGlothlin and Anglin (1981) examined patients from three methadone maintenance treatment programs.
Methadone Dose
In the Ball and Ross studies (1991), patients reduced their use of injected heroin by 71 percent compared with preadmission levels. Illicit opioid use was directly related to methadone dosage: in patients on doses above 71 mg per day, no heroin use was detected, whereas patients on doses below 46 mg per day were 5.16 times more likely to use heroin than those receiving higher doses.
The impact of methadone dose has been demonstrated consistently across studies and countries. Higher (e.g., greater than 50 mg) doses of methadone are associated with better treatment retention and decreased illicit drug use (Faggiano, Vigna-Taglianti, Versino, et al., 2003).
A meta-analysis (Faggiano et al., 2003) of 21 studies concluded that methadone dosages ranging from 60 to 100 mg per day were more effective than lower dosages in retaining patients and in reducing use of heroin and cocaine during treatment.
The following outcomes in the meta-analysis were noted:
Retention rate– randomized clinical trials: high versus low doses at short duration followup: RR = 1.36 [1.13 to 1.63], and at longer duration followup: RR = 1.62 [0.95 to 2.77]
Self-reported opioid use– randomized clinical trials: high versus low doses WMD = -2.00 [4.77 to 0.77], high versus medium doses WMD = -1.89 [-3.43 to -0.35]
Opioid abstinence by urine toxicology at greater than 3 to 4 weeks– randomized clinical trials: high versus low doses RR = 1.59 [1.16 to 2.18], high versus medium doses RR = 1.51 [0.63 to 3.61]
Cocaine abstinence by urine toxicology at greater than 3 to 4 weeks–randomized clinical trials: high versus low doses RR = 1.81 [1.15 to 2.85]
Overdose mortality– high dose versus low dose at 6 years' followup: RR = 0.29 [0.02 to 5.34]; high dose versus medium dose at 6 years' followup: RR = 0.38 [0.02 to 9.34]; medium dose versus low dose at 6 years' followup: RR = 0.57 [0.06 to 5.06]
One study noted lower rates of opioid-positive urine samples (53% vs. 62%, p < .05) in patients who were being treated with 80 to 100 mg of methadone compared with those who were being treated with 40 to 50 mg (Strain et al., 1999).
Counseling Services
Counseling services improve treatment outcomes over the provision of methadone alone (Kraft, Rothbard, Hadley, et al., 1997).
Treatment Duration
In one study, 82 percent of 105 patients who discontinued methadone relapsed to intravenous drug use within 12 months (Payte and Khuri, 1993).
DARP studies of opioid-dependent patients 12 years following admission to treatment showed that illicit opioid use declined progressively over time until year 6, when it stabilized at about 40 percent for “any” use and 25 percent for “daily” use (Simpson, Joe, Lehman, et al., 1986).
In both the DARP and TOPS studies, long treatment duration was the strongest predictor of reduced heroin use among methadone maintenance patients.
Reductions in Illicit Opioid Use During and After Methadone Maintenance Treatment– The DARP and TOPS studies of two different groups of heroin-addicted patients were conducted several years apart. Both demonstrated about a 40-percent reduction in opioid use at the end of 1 year after methadone maintenance treatment.
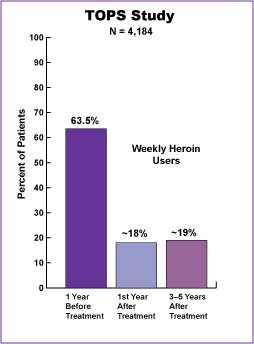
Figure 10 illustrates that, in the TOPS study, almost 64 percent of the patients used heroin at least weekly in the year before treatment; however, about 18 percent used heroin at least weekly in the year after treatment, and about 19 percent continued heroin use weekly 3 to 5 years after (Hubbard, Marsden, Rachal, et al., 1989).
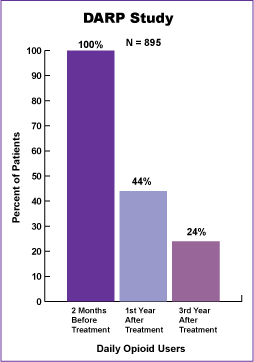
Figure 11 illustrates that in the DARP study, 44 percent of methadone maintenance treatment patients used heroin daily in the year following treatment and 24 percent used heroin daily 3 years after treatment. This represents significant reductions from the 100 percent who had used heroin daily in the 2 months before admission (Simpson and Sells, 1982). Daily illicit opioid use continued to decline steadily for the next 3 years.
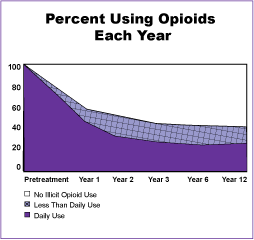
Figure 12 illustrates that improvements among patients who used no illicit opioids and who used opioids less than daily persisted into the 12th year after treatment. About one-half of those patients treated with methadone maintenance reported no illicit drug use after 12 years. The benefits associated with methadone maintenance treatment seem to improve over time. For example, at the end of 1 year, about 50 percent of the subjects reported daily illicit drug use, but by year 12, the proportion using illicit drugs on a daily basis was reduced to about 25 percent (Simpson and Sells, 1990).
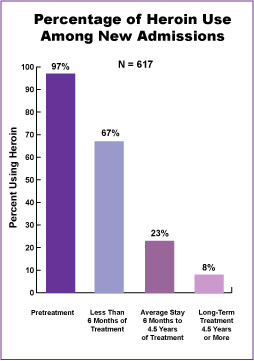
Figure 13 illustrates that heroin use among a group of 617 new admissions was nearly 100 percent. Among patients who stayed in treatment for less than 6 months, about 67 percent reported using heroin. Among patients whose average stay in methadone maintenance treatment was 6 months to 4.5 years, about 23 percent reported using heroin. Among patients who remained in treatment more than 4.5 years, about 8 percent reported using heroin (Ball and Ross, 1991).
References
Amato L, Minozzi S, Davoli M, Vecchi S, Ferri M, Mayet S. Psychosocial combined with agonist maintenance treatments versus agonist maintenance treatments alone for treatment of opioid dependence. The Cochrane Database of Systematic Reviews, Issue 4, 2004.
Ball JC, Ross A. The Effectiveness of Methadone Maintenance Treatment. New York, NY: Springer-Verlag Inc., 1991.
Capelhorn JRM, Bell J. Methadone dosage and retention of patients in maintenance treatment. The Medical Journal of Australia 1991;154:195-99.
Capelhorn JRM, Bell J, Kleinbaum DG, Gebski VJ. Methadone dose and heroin use during maintenance treatment.Addiction 1993;88:119-24.
Condelli WS, Dunteman GH. Exposure to methadone programs and heroin use. American Journal of Drug and Alcohol Abuse 1993;19:65-78.
Faggiano F, Vigna-Taglianti F, Versino E, Lemma P. Methadone maintenance at different dosages for opioid dependence. The Cochrane Database of Systematic Reviews, Issue 3, 2003.
Hubbard RL, Marsden ME, Rachal JV, Harwood HJ, Cavanaugh ER, Ginzburg HM. Drug Abuse Treatment: A National Study of Effectiveness. Chapel Hill: University of North Carolina Press, 1989.
Kraft KM, Rothbard AB, Hadley TR, McLellan AT, Asch DA. Are supplementary services provided during methadone maintenance really cost-effective? American Journal of Psychiatry 1997;154:1214-19.
McLellan AT, Arndt IO, Metzger DS, Woody GE, O'Brien CP. The effects of psychosocial services in substance abuse treatment. JAMA 1993;269(15):1953-59.
Payte JT, Khuri ET. Treatment duration and patient retention. In: State Methadone Treatment Guidelines. Rockville, MD: Center for Substance Abuse Treatment, 1993.
Powers KI, Anglin MD. Cumulative versus stabilizing effects of methadone maintenance. Evaluation Review1993;17(3):243-70.
Simpson DD, Joe GW, Lehman WEK, Sells SB. Addiction careers: etiology, treatment, and 12-year follow-up outcomes. Journal of Drug Issues 1986;16(1):107-21.
Simpson DD, Sells SB. Effectiveness of treatment for drug abuse: an overview of the DARP research program.Advances in Alcohol and Substance Abuse 1982;2(1):7-29.
Simpson DD, Sells SB (eds.). Opioid Addiction and Treatment: A 12-Year Follow-Up. Malabar, FL: Krieger Publishing Company, 1990.
Strain EC, Bigelow GE, Liebson IA, Stitzer ML. Moderate- vs high-dose methadone in the treatment of opioid dependence. A randomized trial. JAMA 1999;281:1000-05.
Strain EC, Stitzer ML, Liebson IA, Bigelow GE. Dose-response effects of methadone in the treatment of opioid dependence. Annals of Internal Medicine 1993;119:23-37
In This Section
- Certificate Programs
- Methadone Research Web Guide
- Acknowledgments
- Introduction
- Part A
- Part B
- Question 1: Is methadone maintenance treatment effective for opioid addiction?
- Question 2: Does methadone maintenance treatment reduce illicit opioid use?
- Question 3: Does methadone maintenance treatment reduce HIV risk behaviors and the incidence of HIV infection among opioid-depen
- Question 4: Does methadone maintenance treatment reduce criminal activity?
- Question 5: Does methadone maintenance treatment improve the likelihood of obtaining and retaining employment?
- Question 6: What effect can methadone maintenance treatment have on the use of alcohol and other drugs?
- Question 7: What components of methadone maintenance treatment account for reductions in AIDS risk behaviors?
- Question 8: Do risk factors for HIV infection acquisition and transmission differ for women compared with men in methadone maint
- Question 9: Is methadone maintenance treatment effective for women?
- Question 10: Is methadone safe for pregnant women and their infants?
- Question 11: Is it necessary to reduce methadone dose or detoxify women from methadone during pregnancy to protect the f
- Question 12: Is the long-term use of methadone medically safe, and is it well tolerated by patients?
- Question 13: Are there program characteristics associated with the success of methadone maintenance treatment?
- Question 14: Are there patient characteristics associated with the success of methadone maintenance treatment?
- Question 15: Are there cost benefits to methadone maintenance treatment?
- Question 16: What are the retention rates for methadone maintenance treatment?
- Question 17: Is mandated methadone maintenance treatment as effective as voluntary treatment?
- Question 18: What is the role of L-alpha-acetyl-methadol (LAAM)?
- Question 19: How do buprenorphine and methadone compare?
- Question 20: Can methadone and buprenorphine be abused?
- Part C
- Part D
- Methadone Research Web Guide Tutorial
- Questions: Methadone Research Web Guide
- Answers: Methadone Research Web Guide
- Methadone Research Web Guide
- Degree Programs
- Virtual Lectures
- Research Publications
Important Dates
NIDA International Forum
June 14–17, 2013
Online Registration Deadline:
May 6, 2013
FELLOWSHIPS
IAS/NIDA Fellowships
Application Deadline:
February 10, 2013
NIDA International Program Fellowships
Application Deadline:
April 1, 2013
Global Health Program for Fellows and Scholars
Application Deadlines: Vary
GRANTS
Brain Disorders in the Developing World: Research Across the Lifespan
(Non-AIDS)
R01 PAR-11-030and R21 PAR-11-031
Application deadline:
February 14, 2013
MEETINGS
American Association for the Advancement of Science
February 14–18, 2013
Boston, Massachusetts, USA
International Drug Abuse Research Society (IDARS)
April 15–19, 2013
Mexico City, Mexico
2013 International Conference on Global Health: Prevention and Treatment of Substance Abuse and HIV
April 17–19, 2013
Taipei, Taiwan
Yih-Ing Hser, Ph.D.

.png)


